Multifocal Choroiditis And Panuveitis (MFCPU) – April, 2022

History
A 54-year-old woman presented to our clinic for evaluation of possible age-related macular degeneration (AMD) with choroidal neovascular membrane of the left eye. The referring physician recommended injecting the left eye with anti-VEGF injections to treat wet AMD. The patient had noted intermittent blurry vision of the left eye for a few months, with associated headaches and floaters.
Exam
On exam, the patient had count fingers vision in the left eye and 20/20 vision in the right eye. She had intraocular pressures of 10 in the right eye and 16 in the left eye. There was a mild afferent pupillary defect of the left eye. There were retinal pigmentary changes and drusen in both maculae. The left eye had more extensive pigmentary atrophy centrally. Fundus photos were taken as seen on Figure 1.
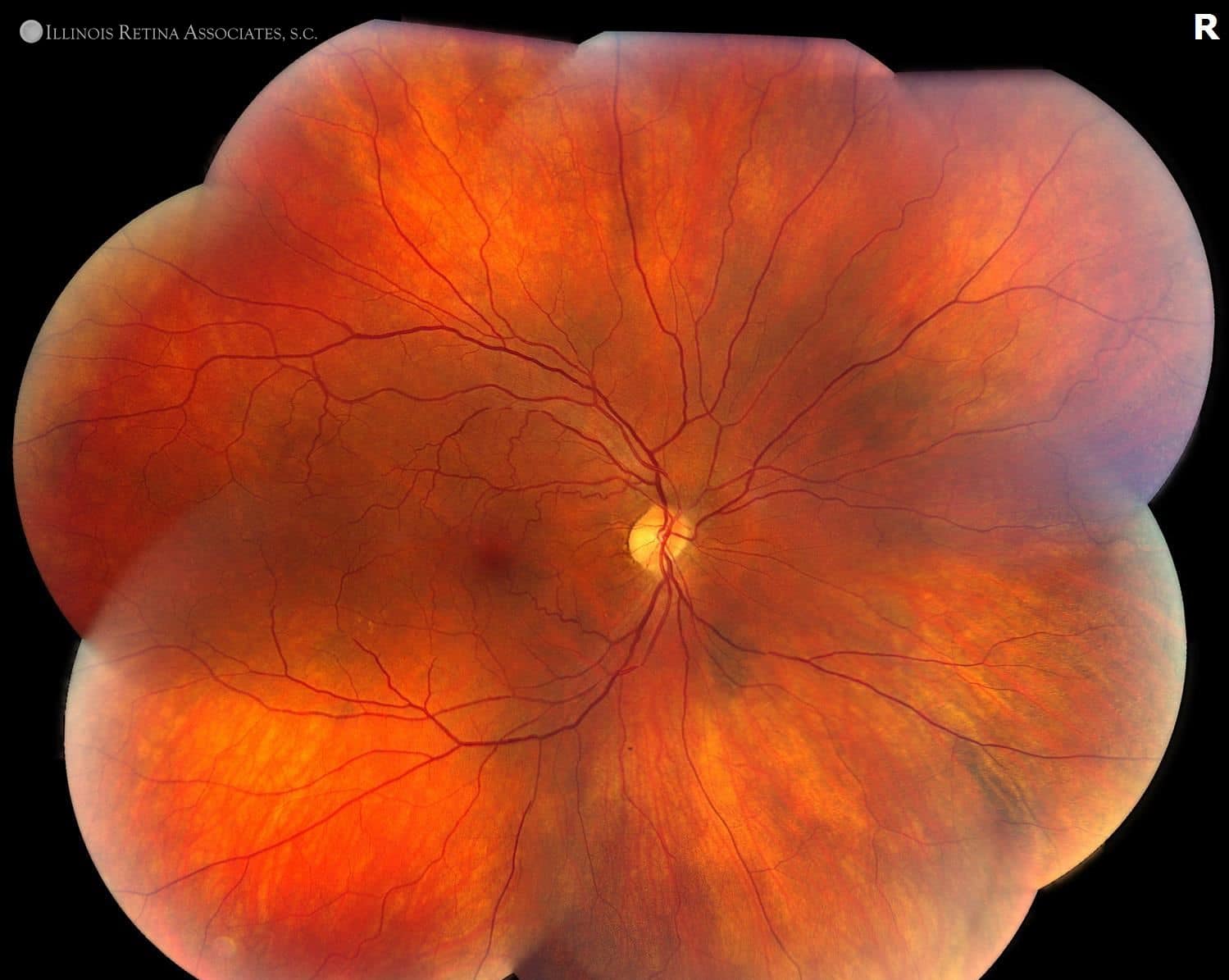
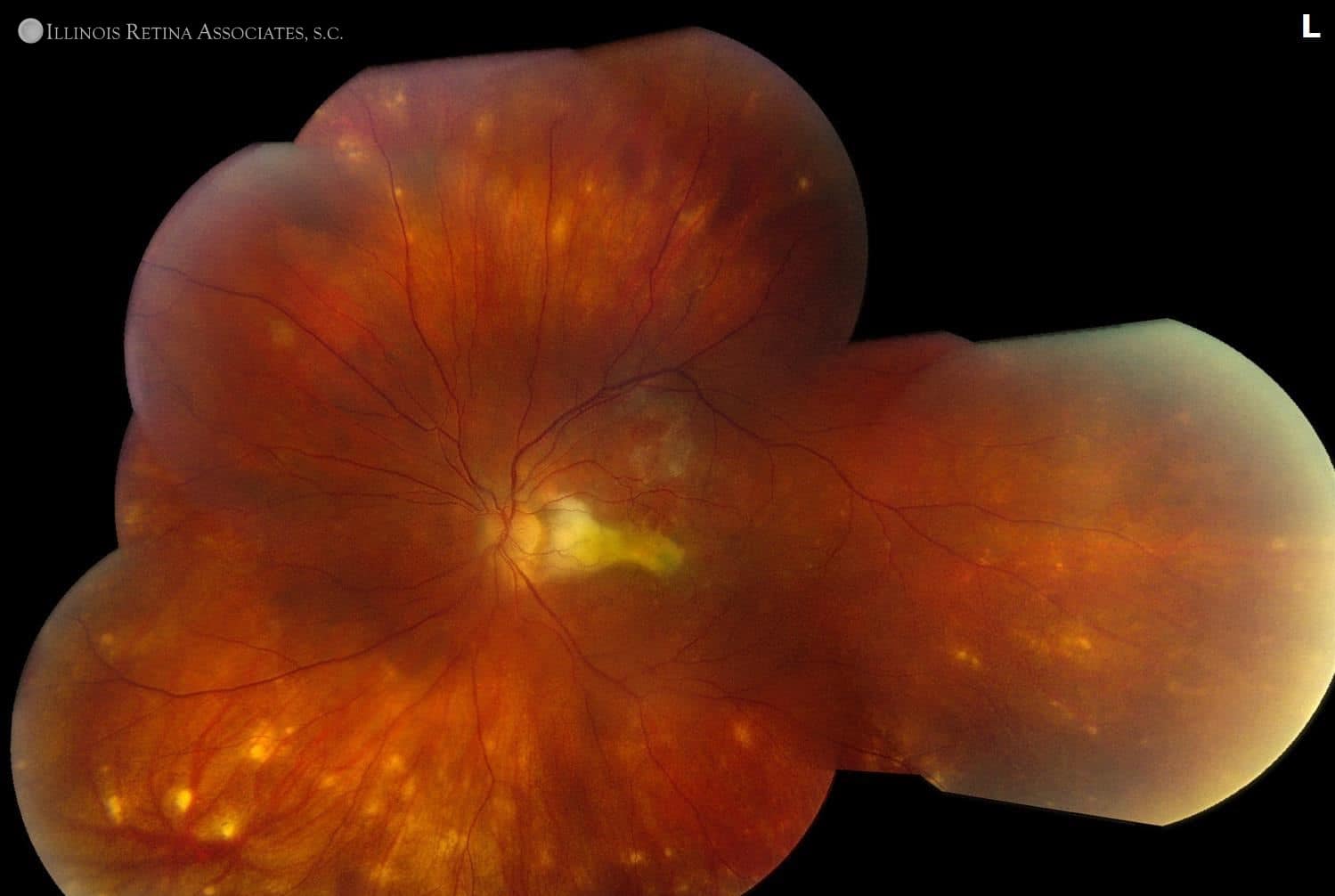
Figure 1. Fundus montages of the right and left eyes. Both eyes show posterior pigmentary change, however there are significantly more in the left eye. Additionally, peripheral white-yellow lesions are scattered throughout the fundus in the left eye.
In order to better characterize the disease, especially in the context of the asymmetry and peripheral lesions of the left eye, fundus autofluorescence (Figure 2), fluorescein angiography (Figure 3), and indocyanine green angiography (Figure 3) were obtained.
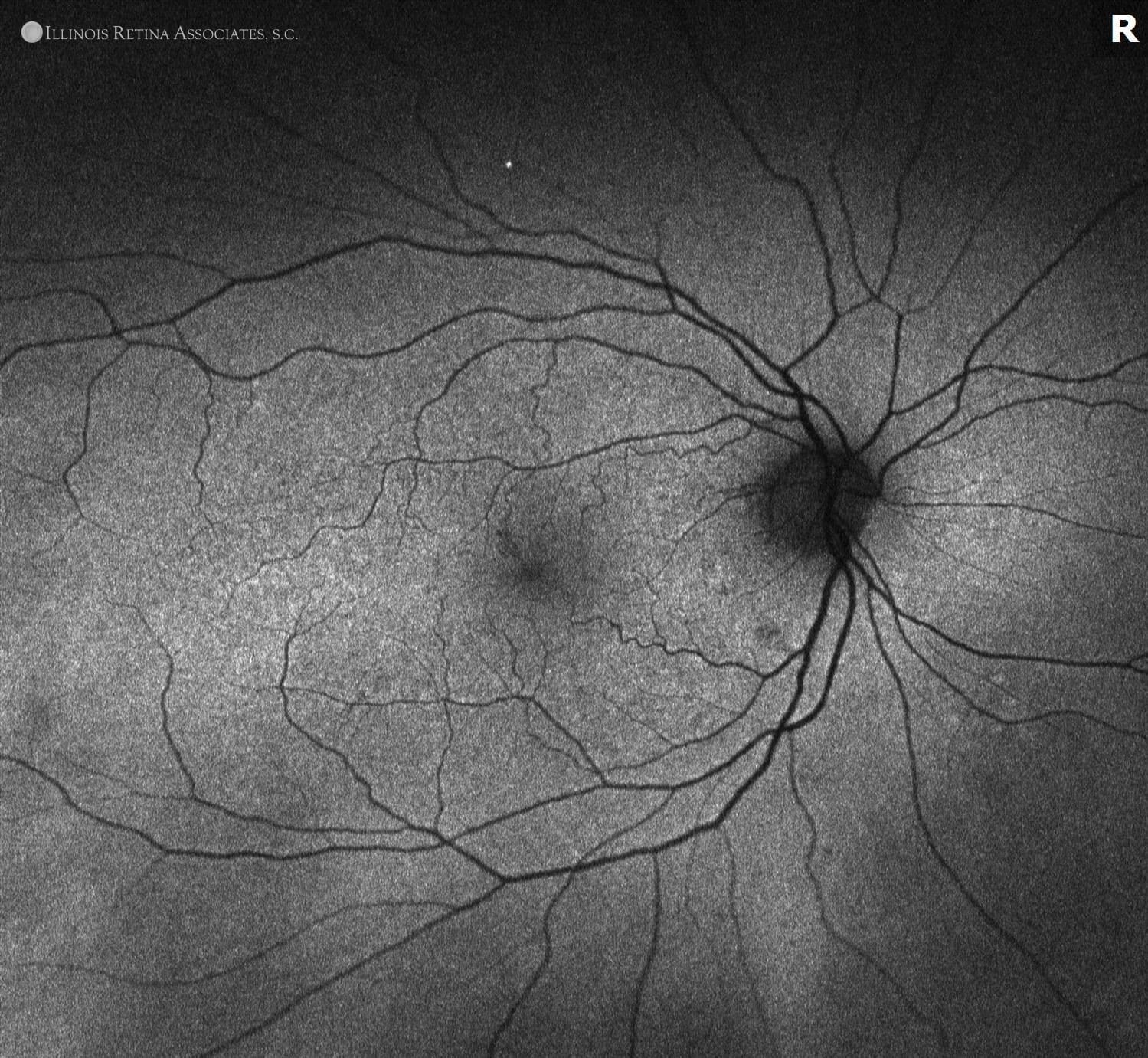
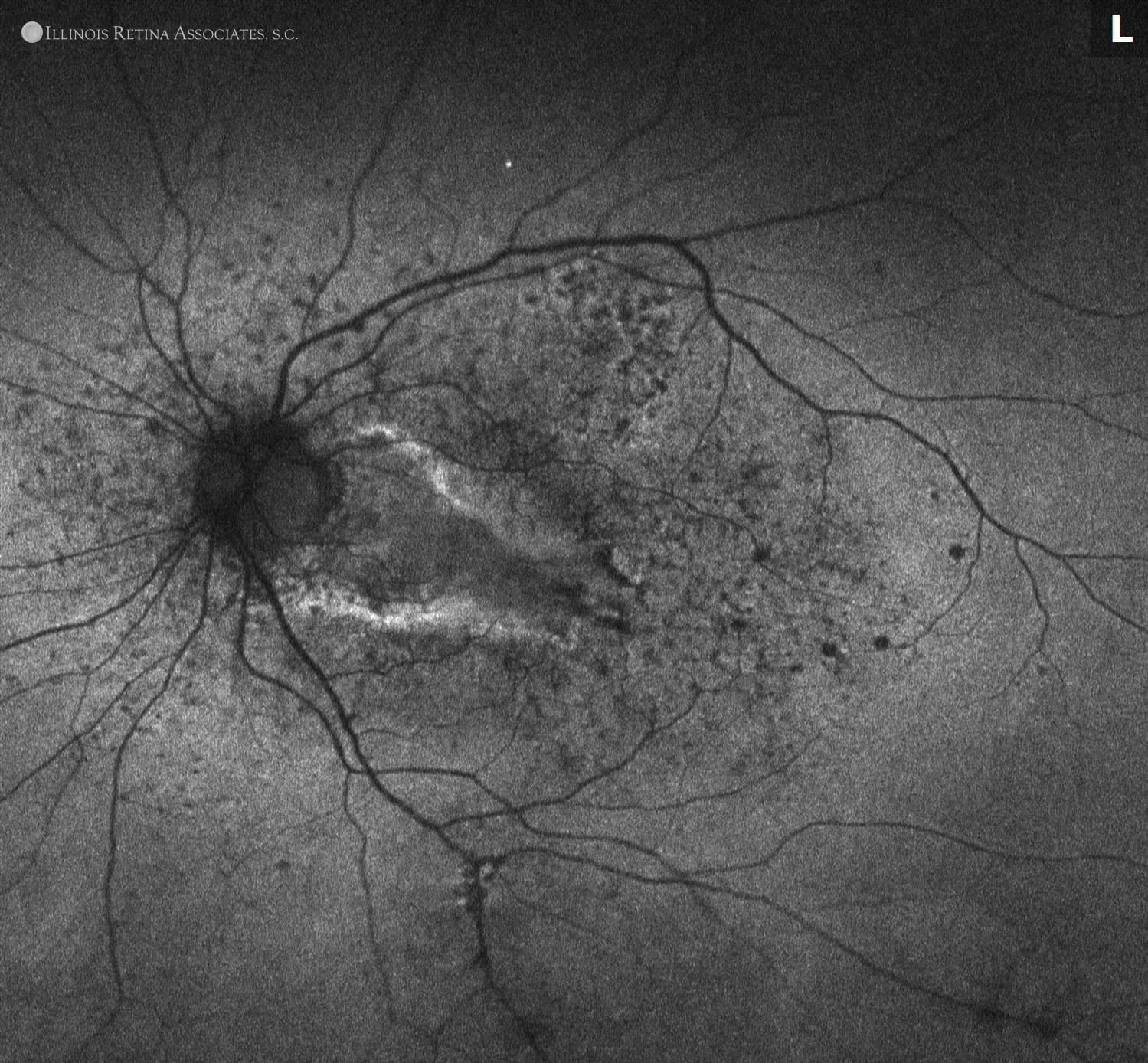
Figure 2. Fundus autofluorescence of the right eye was consistent with drusen, and mixed hyper- and hypo-autofluorescence of the left eye consistent with active and inactive subretinal fibrosis.
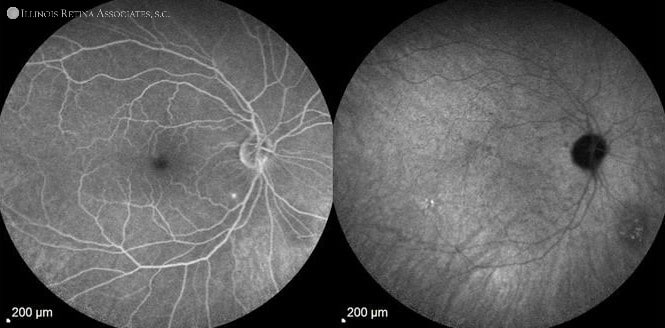
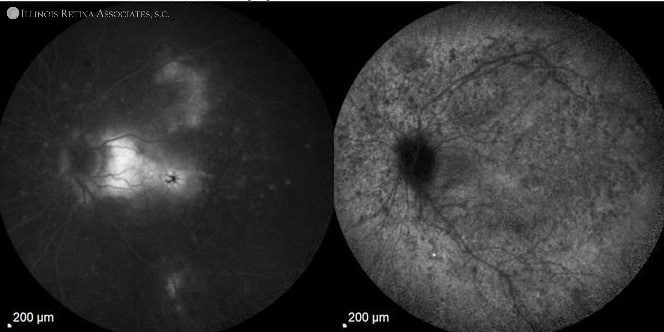
Figure 3. Fluorescein angiography (FA) with indocyanine green angiography (ICG) of the right eye show late staining of the drusen on FA and hypocyanescence inferonasal to the nerve consistent with a choroidal lesion of unknown significance on ICG. The left eye FA show early staining of likely subretinal fibrosis and late leakage of cystoid macular edema with ICG show multiple hypocyanescent lesions of the choroid.
At this point, additional history was elicited from the patient in the context of the peripheral lesions, asymmetry of disease, and the extensive scarring of the left eye in a pattern atypical for AMD. Patient endorsed having sudden loss of vision 1 year prior and was referred with possible optic neuritis or ischemic optic neuropathy to a neuro-ophthalmologist. She missed her follow-up appointments and then noticed additional significant vision loss. She then was seen by her comprehensive ophthalmologist who noted the retinal lesions and sent her to our office.
Differential Diagnosis:
- Neovascular age-related macular degeneration
- Presumed ocular histoplasmosis syndrome (POHS)
- Punctate inner choroidoapathy (PIC)
- Multifocal choroiditis and panuveitis (MFCPU)
- Serpiginous choroiditis
- Tuberculous choroiditis
- Sarcoidosis
- Neuroretinitis
- Placoid syphilitic retinitis
Clinical Course:
Additional lab testing for sarcoidosis, syphilis, Lyme, toxoplasma, toxocara, tuberculosis, and Bartonella were unremarkable. Prior notes documented history of moderate vitreous inflammation which would be atypical for POHS and the size of the peripheral white dots was unusual for PIC. The bilaterality pointed more towards MFCPU, which became the leading diagnosis.
Local and systemic treatment was started with oral steroids and Ozurdex injections. The inflammation improved and the subretinal fibrosis in the macula stopped progressing. The patient was also switched to steroid sparing immunosuppressive therapy of methotrexate and she is doing well. Her right eye vision has been preserved, and monocular precautions were advised.
Discussion:
Multifocal choroiditis and panuveitis (MFCPU)
MFCPU is an idiopathic, inflammatory disease in which patients present with multiple chorioretinal lesions. The disease causes bilateral inflammation that can be asymmetric. For this “white dot syndrome,” the “white dots” are much larger than those seen in PIC and there is usual vitritis as opposed to POHS. Almost all white dot syndromes can result in choroidal neovascular membranes, and treatment can prevent vision loss.
While there is no etiology known at present, infectious causes must be ruled out prior to treatment with steroids. Once the diagnosis is made, treatment can be individualized and must be fastidious to prevent bilateral vision loss. This case highlights the importance of early referral to a retina specialist.
If you are looking to schedule your first consultation, please contact us today by clicking HEREand find the location that is nearest you!
References:
- Essex, Rohan W., et al. “Idiopathic Multifocal Choroiditis.” Retina, vol. 33, no. 1, 2013, pp. 1–4., doi:10.1097/iae.0b013e3182641860.
- Goldstein, Debra, and Lary Ulanski. “Multifocal Choroiditis vs. PIC: Variations on a Theme?” Review of Ophtalmology, 2004.
- Pinar, Vakur, and Stephen Foster. “Bilateral Chorioretinal Lesions Appearing Late in Posterior Uveitis.” 2000.
- Dolz-Marco, Rosa, et al. “How to Differentiate Myopic Choroidal Neovascularization, Idiopathic Multifocal Choroiditis, and Punctate Inner Choroidopathy Using Clinical and Multimodal Imaging Findings.” Ophthalmic Surgery, Lasers and Imaging Retina, SLACK Incorporated, 16 Mar. 2017,
- Li, J., Li, Y., Li, H. et al. Imageology features of different types of multifocal choroiditis. BMC Ophthalmol 19, 39 (2019). https://doi-org.ezproxy.med.ucf.edu/10.1186/s12886-019-1045-x
