Toxoplasmosis Chorioretinitis – June, 2022

History:
A 41-year-old Jamaican man presented to our clinic for evaluation of new floaters in the left eye. He described having such floaters intermittently in both eyes over a period of 5-10 years, sometimes associated with a dull ache. This time, the floaters were blurring his vision in the left eye, though the right eye was not having any issues. He also had a mild headache, which he attributed to the blurry vision.
Exam:
On exam, the patient had hand motion vision in the left eye and 20/20 vision in the right eye. He had an IOP of 14 in the right eye and 21 in the left eye. There was no afferent pupillary defect, however on confrontational visual fields, there was superior and temporal loss in the left eye. On further exam of the left eye, the anterior chamber and vitreous each had 2+ cell. Fundus photos were taken (Figure 1).
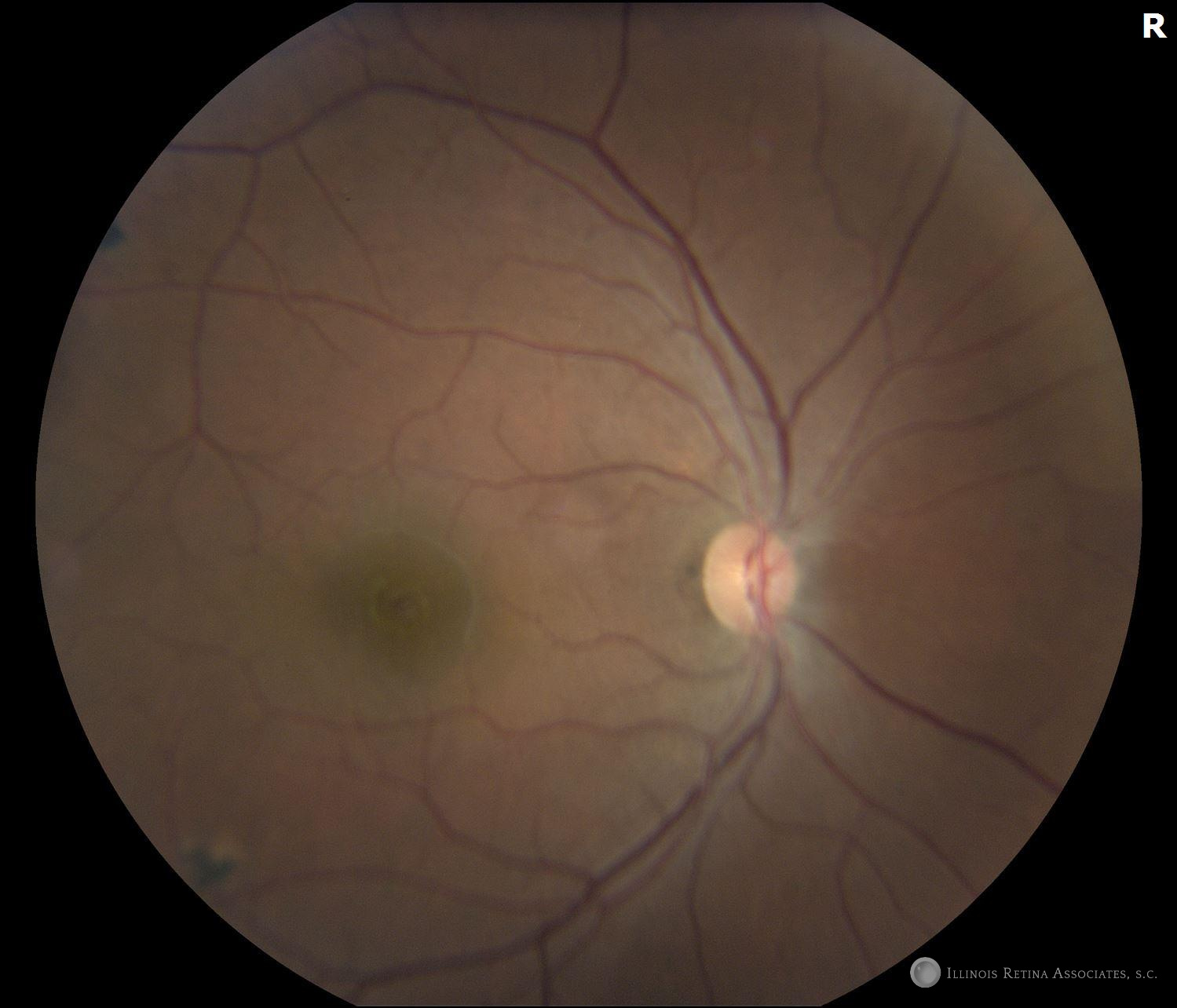
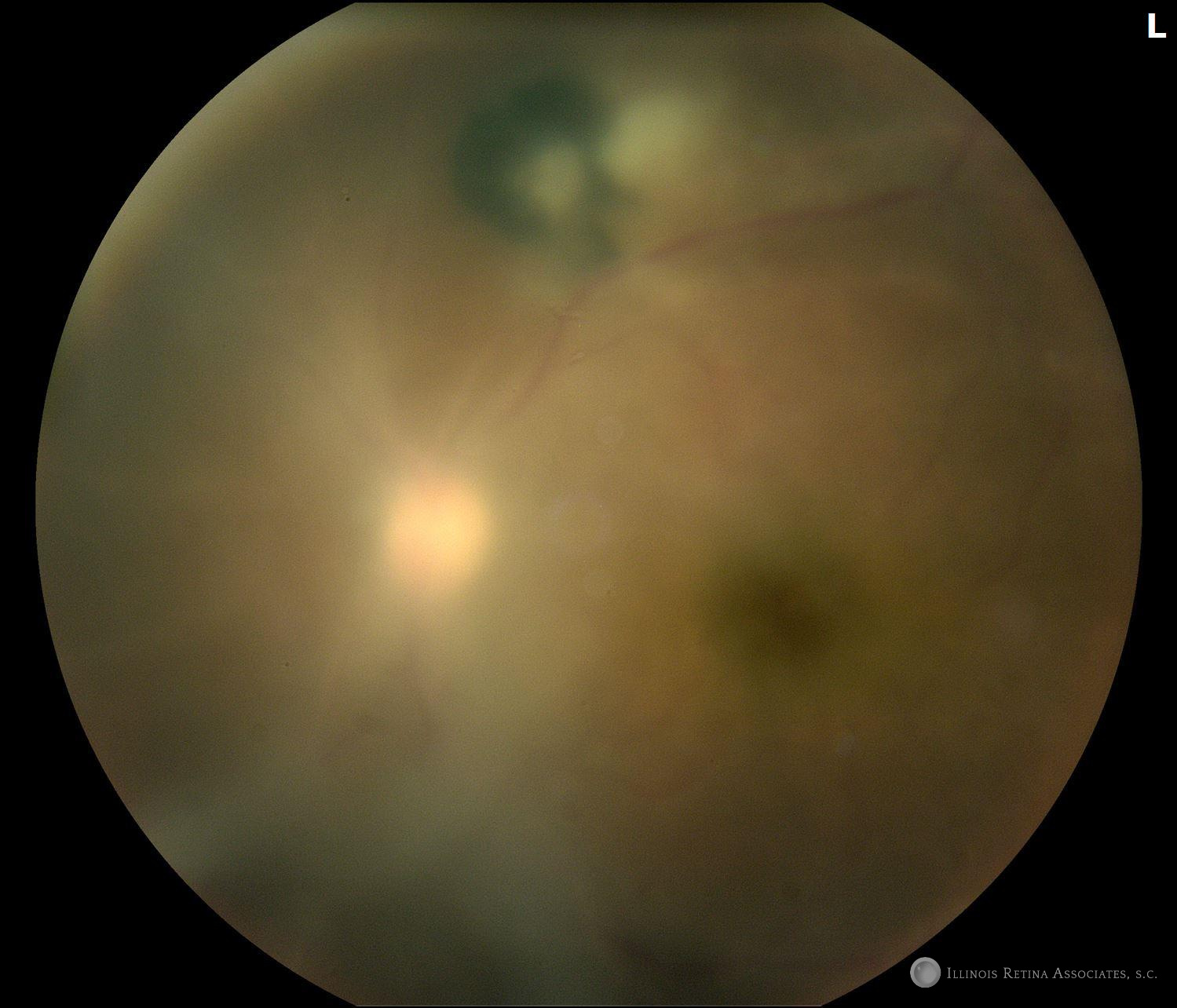
Figure 1. Color fundus photos of the right and left eyes. Both eyes showed chorioretinal scars. These were more pronounced in the left eye. Additionally, the left eye has media opacities and fluffy white infiltrates overlying the chronic hyperpigmented scars.
To better characterize the disease, fluorescein angiogram was obtained (Figure 2).
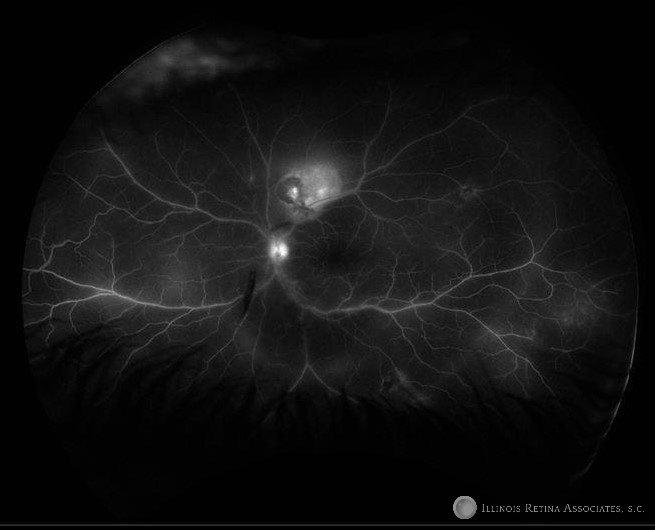
Figure 2. Fluorescein angiogram demonstrates hyperfluorescence neighboring the window defect of chorioretinal scarring consistent with chronic scarring with associated acute, active chorioretinitis. Additionally perivascular hyperfluorescence is visible both along the arcades and periphery consistent with an acute vasculitis. Media opacities resulting in blocking type of hypofluorescence are visible due to the overlying vitritis.
At this point, additional history was elicited from the patient in the context of the peripheral lesions, asymmetry of disease, and the extensive scarring of the left eye. Patient reported having grown eating a variety of fresh fish and meats in Jamaica.
Differential Diagnosis:
- Toxoplasmosis chorioretinitis
- Tuberculosis
- HIV Retinitis
- Toxocariasis
- Sarcoidosis
- Syphilis
- Cytomegalovirus retinitis
- Candida endophthalmitis
- Punctate inner choroidopathy (PIC)
- Multifocal choroiditis (MFC)
- Presumed Ocular Histoplasmosis (POHS)
Clinical Course:
Additional lab testing was obtained. Toxoplasmosis antibody titers were positive for IgG, though negative for the acute antibody titer IgM. Tuberculosis and syphilis testing was performed and negative. Testing for sarcoidosis, Lyme, Toxocara, and Bartonella were all normal.
In terms of non-infectious etiologies, the moderate vitreous inflammation would be atypical for POHS. The size of the peripheral white dots was unusual for PIC. The character of the lesions was less likely MFC.
The patient was started on oral Bactrim and topical prednisolone acetate to treat presumptive toxoplasmosis chorioretinitis. A few days after starting the antibiotic, his infection improved, and he was started on oral Prednisone to address inflammation. His vitritis continued to resolve, and within a week his inflammation had subsided. His vision improved to 20/40, and he began a steroid taper while still under the cover of Bactrim to prevent a recurrence of active infection.
Discussion:
Toxoplasmosis chorioretinitis
Our patient demonstrated the classic clinical presentation for toxoplasmosis of “headlight in the fog,” describing vitritis overlying a chorioretinal infiltrate. Toxoplasmosis is the most common cause of posterior uveitis in the world. Risk factors for the disease include owning cats or eating raw or undercooked meat or fish. Prevalence is highest in tropical climates and lowest in dry and colder climates. Incidence is high in Jamaica, where our patient was born. It is common for the infection to be indolent for many years and reactivate later in life as in our patient’s case.
Fortunately, multiple antibiotic regimens exist for treatment of toxoplasmosis chorioretinitis. Patients often respond well to oral Bactrim with or without topical and systemic steroids. Triple therapy with pyrimethamine, sulfadiazine, and folinic acid is also an option, though the cost may be prohibitive. Recalcitrant or severe cases may be treated with the addition of intravitreal clindamycin injection as well. Other treatment options include systemic clindamycin or azithromycin. Mild peripheral cases may be observed unless a patient is pregnant, monocular, or immunocompromised. Meanwhile posterior cases as in our patient are often treated more aggressively.
Without treatment, toxoplasmosis can be a devastating, blinding disease. With earlier evaluation and intervention by a retinal or uveitis specialist, even despite macular involvement, a significant portion of baseline vision can often be retrieved.
If you are looking to schedule your first consultation, please contact us today by clicking HERE and find the location that is nearest you!
References:
- Jones JL, Dargelas V, Roberts J, Press C, Remington JS, Montoya JG. Risk factors for Toxoplasma gondii infection in the United States. Clin Infect Dis. 2009 Sep 15;49(6):878-84. doi: 10.1086/605433. PubMed PMID: 19663709.
- Bosch-Driessen LH, Plaisier MB, Stilma JS, Van der Lelij A, Rothova A. Reactivations of ocular toxoplasmosis after cataract extraction. Ophthalmology. 2002 Jan;109(1):41-5. PubMed PMID: 11772577.
- Kim SJ, Scott IU, Brown GC, Brown MM, Ho AC, Ip MS, Recchia FM. Interventions for toxoplasma retinochoroiditis: a report by the American Academy of Ophthalmology.Ophthalmology. 2013 Feb;120(2):371-8. doi: 10.1016/j.ophtha.2012.07.061. Epub 2012 Oct 11. Review. PubMed PMID: 23062648.
