Angioid Streaks – July, 2022

History:
A 50-year-old woman was referred by an Optometrist for macular changes in both eyes. She had been followed for a retinal condition that her sister also has since her early 20s. The patient has noted distorted vision in her left eye for about 2-3 weeks. Her past medical history was significant for asthma. Other than her sister there are no other affected family members. Review of systems was positive for characteristic skin changes on her neck.
Exam:
Her visual acuity was 20/30 PHNI in both eyes. There was no RAPD. Intraocular pressures were 13 and 14 in the right and left eyes, respectively. Anterior segment exam demonstrated trace nuclear sclerosis in both eyes. Dilated fundus examination demonstrated many peripapillary hyperpigmented subretinal streaks emanating from the optic nerve in both eyes with a small amount of subretinal fluid in each macula and pigmentary changes. There was no hemorrhage seen.
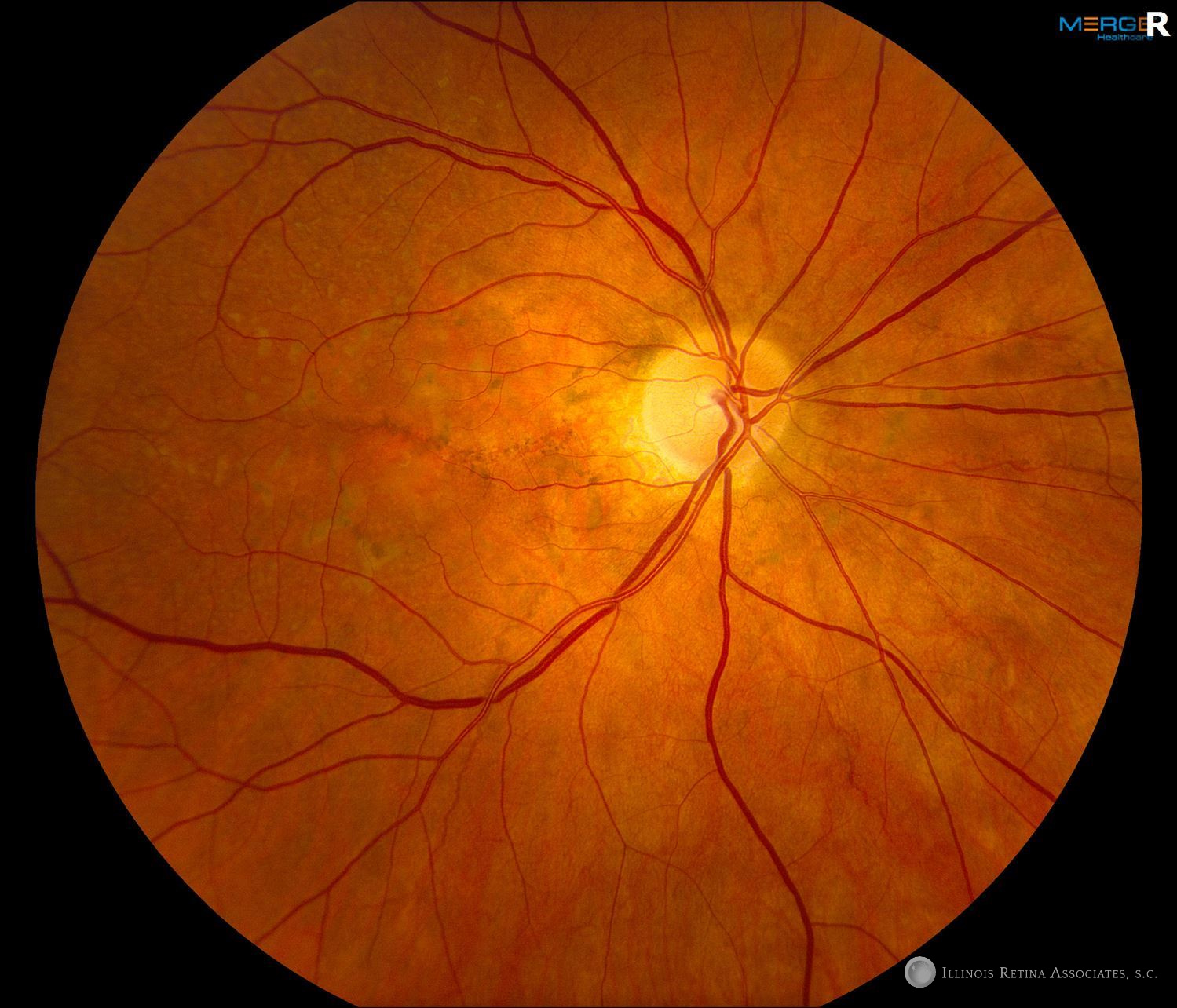
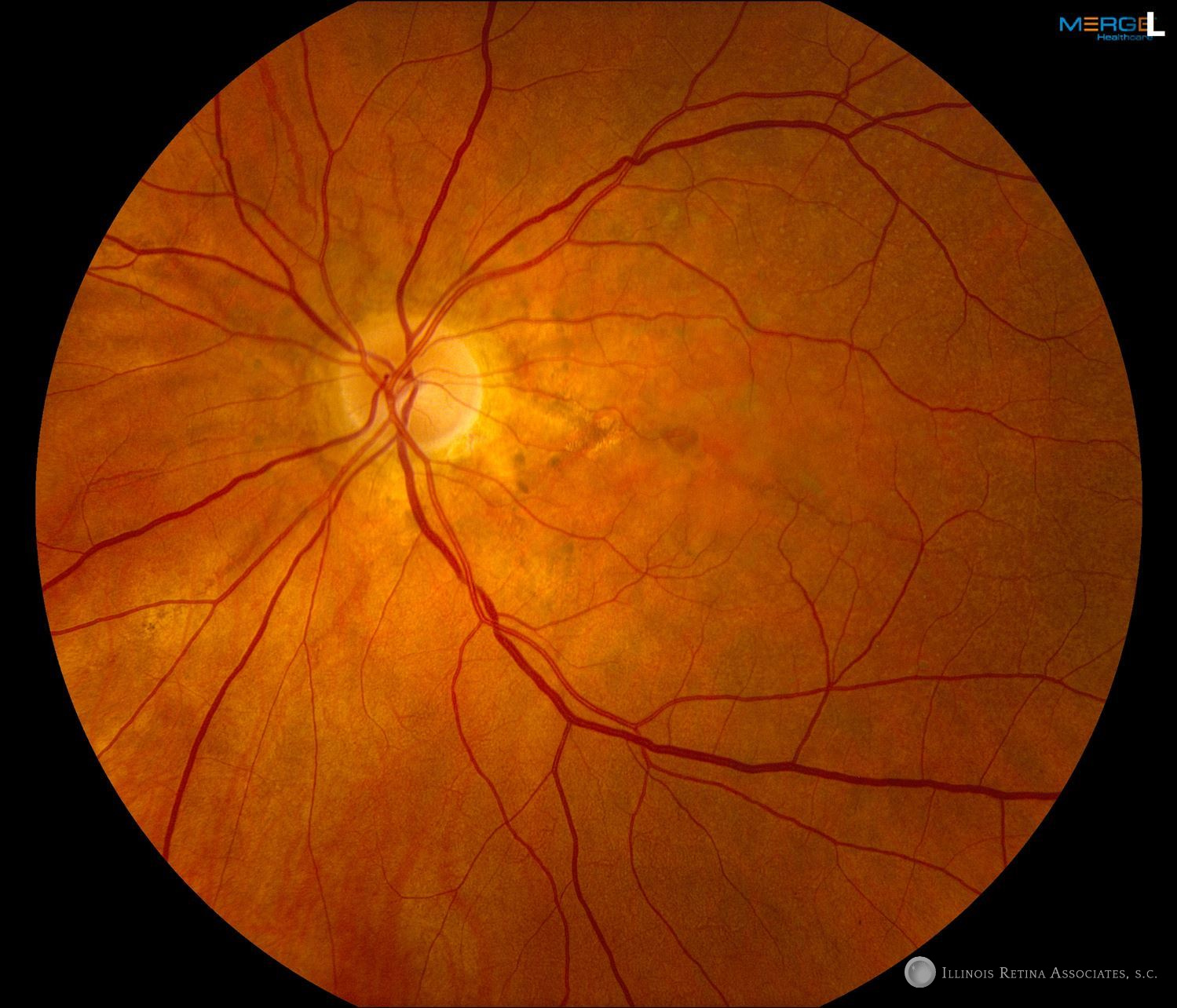
Figure 1: Fundus photographs of the right and left eye demonstrating angioid streaks and subretinal fluid.
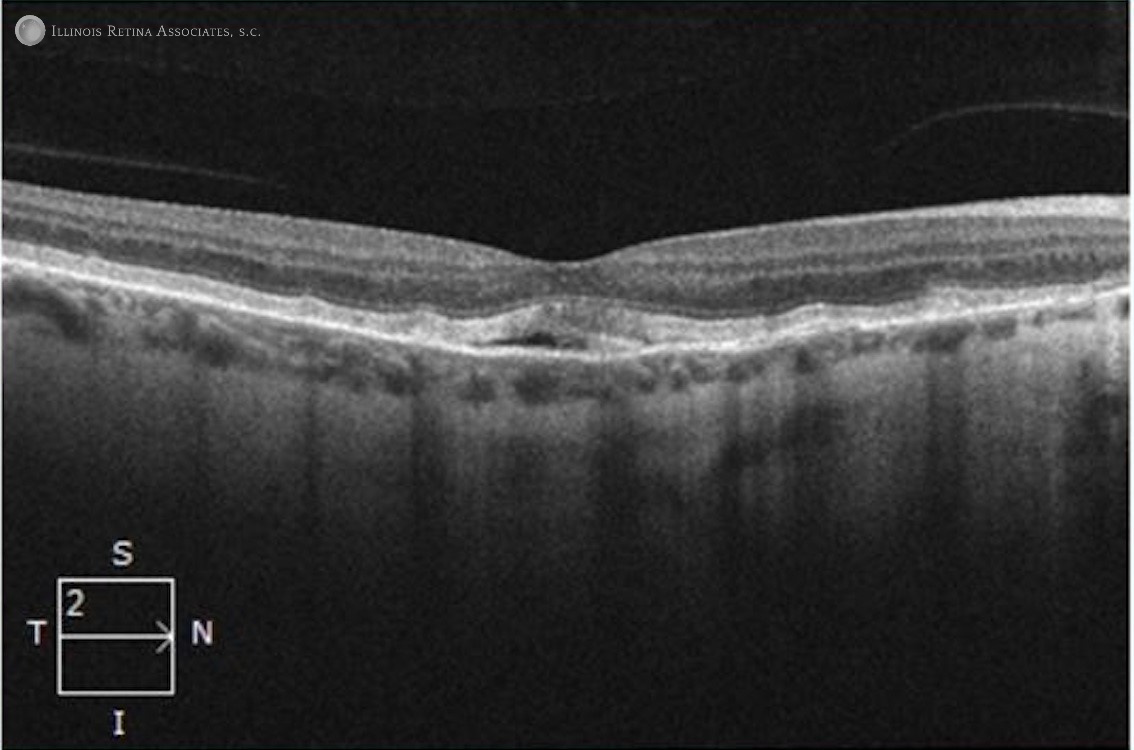
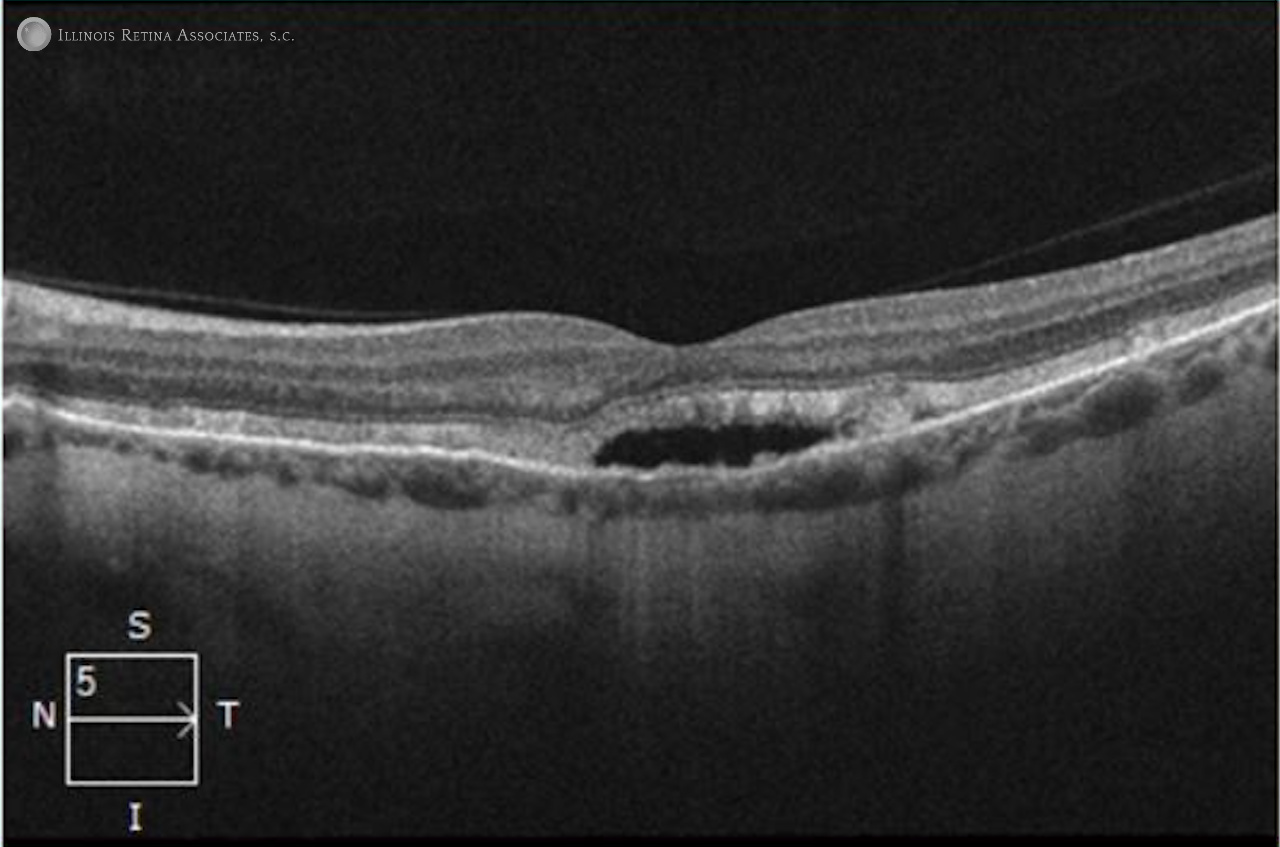
Figure 2: Optical Coherence Tomography (OCT) scans of the right and left eye, respectively, showed the presence of subretinal fluid.
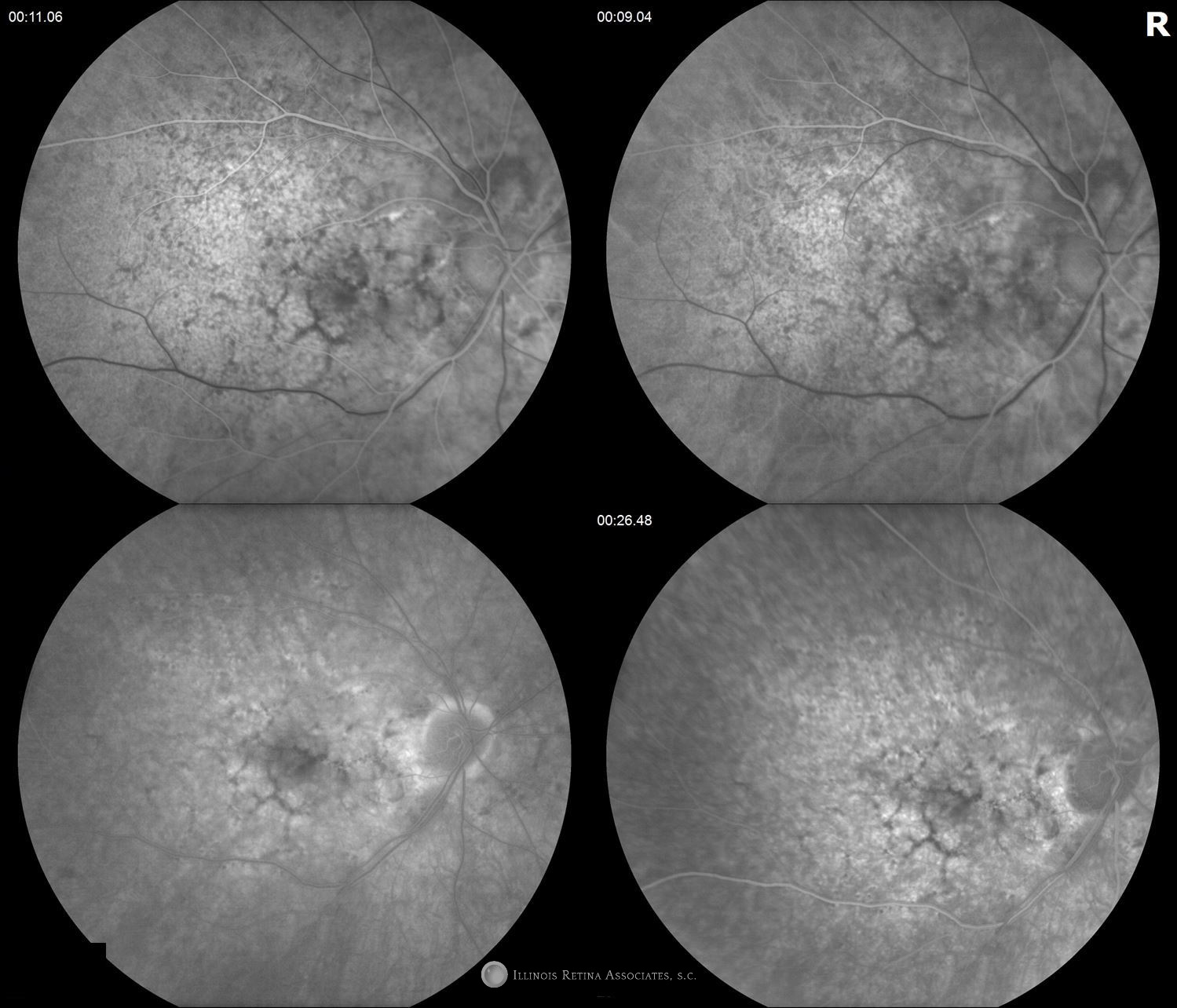
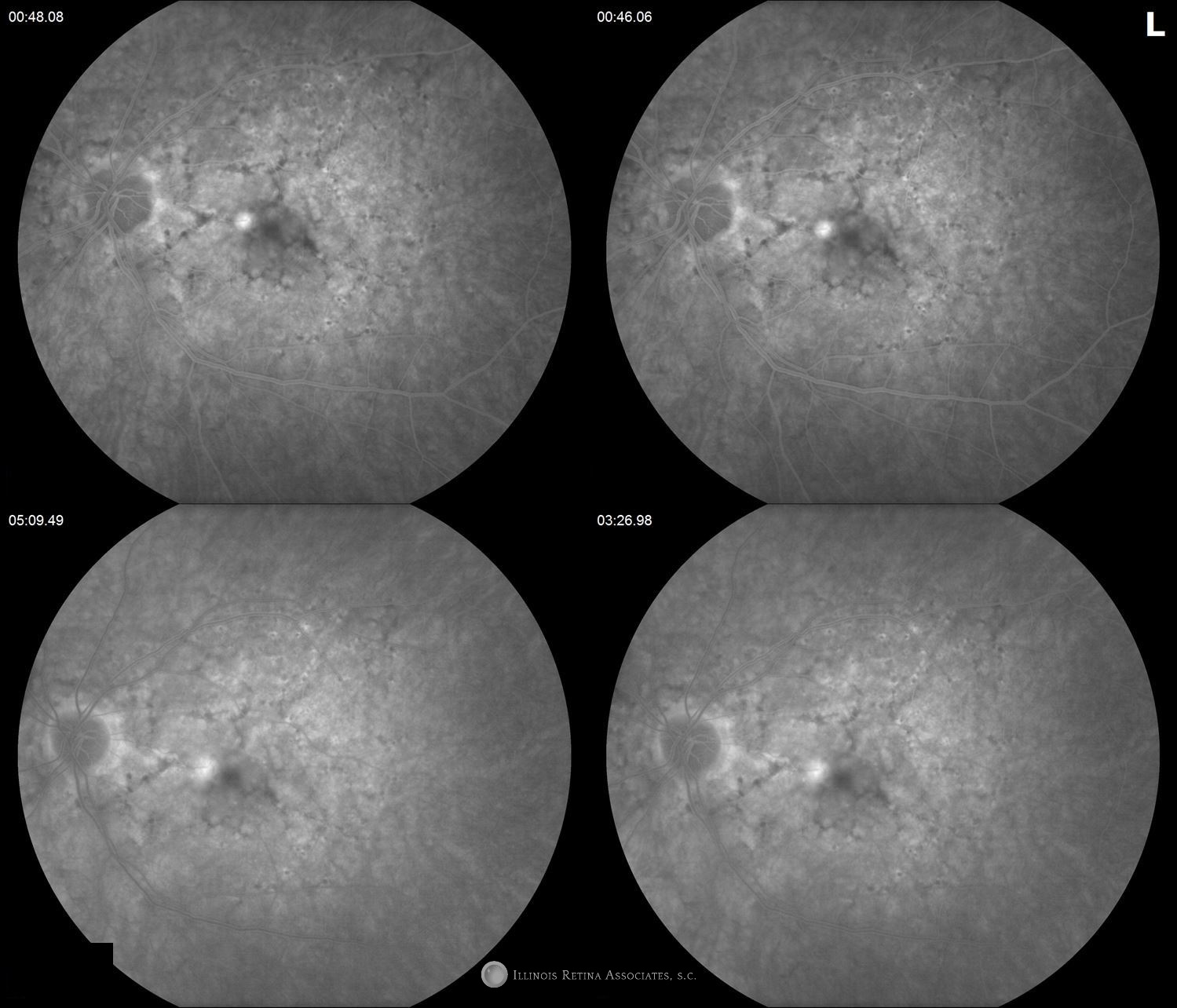
Figure 3: Intravenous fluorescein angiography demonstrated transmission defects consistent with RPE atrophy and late leakage from an undetermined source in the right eye (occult CNV) with early hyperfluorescence (classic CNV) in the left eye.
Differential Diagnosis:
- Angioid streaks
- Pattern dystrophy
- Age related macular degeneration
- Lacquer cracks (pathologic myopia)
- Choroidal rupture
Discussion:
Angioid Streaks
Angioid streaks is a bilateral condition characterized by irregular narrow lines deep to the retina that radiate from the optic disc. They represent a weakened Bruch’s membrane. Angioid streaks are associated with numerous systemic diseases most commonly pseudoxanthoma elasticum. Other systemic associations include Ehler-Danlos syndrome, Paget disease of the bone, Sickle cell disease, and other hemoglobinopathies. Additionally, they may be idiopathic. Although the exact pathogenesis is unknown, studies have shown extensive calcification which predisposes Bruch’s membrane to cracks and rupture. This can lead to subretinal hemorrhage, choroidal neovascularization, and disciform scarring. Due to this predisposition to rupture, patients are encouraged to wear rigid eye protection to prevent accidental blunt trauma.
Diagnosis can be made on clinical exam alone based on the characteristic streaks. Fluorescein angiogram can be helpful to diagnose an associated choroidal neovascular membrane. When a choroidal neovascular membrane is diagnosed intravitreal anti-VEGF treatment is the mainstay and typically offers good results.
Often more important is the systemic work up of the patient when patients are newly diagnosed without a known systemic cause. The medical work up should be tailored to the patient based on a review of systems. This is usually performed by an internist with the most common associations being pseudoxanthoma elasticum, Paget disease of the bone, and sickle cell hemoglobinopathies.
Our patient had a genetically confirmed diagnosis of pseudoxanthoma elasticum (ABCC6) and her skin changes were typical of the small, yellowish papular lesions that often affect the neck and flexural creases. After an initial series of 3 monthly intravitreal injections, her fluid resolved, and vision returned to 20/20 in each eye. She has been subsequently maintained on a treat and extend regimen with preservation of her visual acuity.
If you are looking to schedule your first consultation, please contact us today by clicking HERE and find the location that is nearest you!
References:
- Finger RP, Charbel Issa P, Ladewig MS, Götting C, Szliska C, Scholl HP, Holz FG (2009). “Pseudoxanthoma elasticum: genetics, clinical manifestations and therapeutic approaches”. review. Survey of Ophthalmology. 54 (2): 272–85.
- Stumpf MJ, Mahn T, Steinmetz M, Fimmers R, Pizarro C, Nickenig G, et al. Pseudoxanthoma elasticum- also a microvascular disease. 2020;49(1):57-62.
- Uitto J, Jiang Q, Varadi A, Bercovitch LG, Terry SF. Pseudoxanthoma elasticum: diagnostic features, classification, and treatment options. Expert Opin Orphan Drugs. 2014;2(6):567-577.
- Bercovitch L, Terry P. Pseudoxanthoma elasticum 2004. J Am Acad Dermatol. 2004;51(1 Suppl):S13–4.
- Gliem M, Müller PL, Birtel J, Hendig D, Holz FG, Charbel Issa P. Frequency, phenotypic characteristics and progression of atrophy associated with a diseased bruch’s membrane in pseudoxanthoma elasticum. Invest Ophthalmol Vis Sci. 2016;57:3323–30.
- Gliem M, Birtel J, Muller P, Hendig D, Faust I, Herrmann P, et al. Acute retinopathy in pseudoxanthoma elasticum. JAMA Ophthalmol.2019;237(10):1165-1173.

