Hypertensive Retinopathy – January 2021

History
A 38-year-old male with hypertension and diabetes presented to clinic referred by an optometric colleague for evaluation of decreased vision and a hemorrhages of the left retina. He had noticed a sudden decrease in vision in the left eye more so than the right eye since last week. He was in the hospital the week prior due to uncontrolled high blood pressure (about 230/130). He just started taking medications for hypertension a few days prior to his retinal evaluation.
Exam
On exam, his vision was about 20/60 and IOP was 20 in the left eye. The right eye was 20/20 with an IOP of 19. Confrontation visual fields were full bilaterally. Anterior chambers were Deep and Quiet. Evaluation of his posterior segment demonstrated both maculas having macular edema, hard exudates, and moderate dot/blot hemorrhages (DBHs) as well as cotton wool spots (CWSs). Below are his color fundus photo montages:
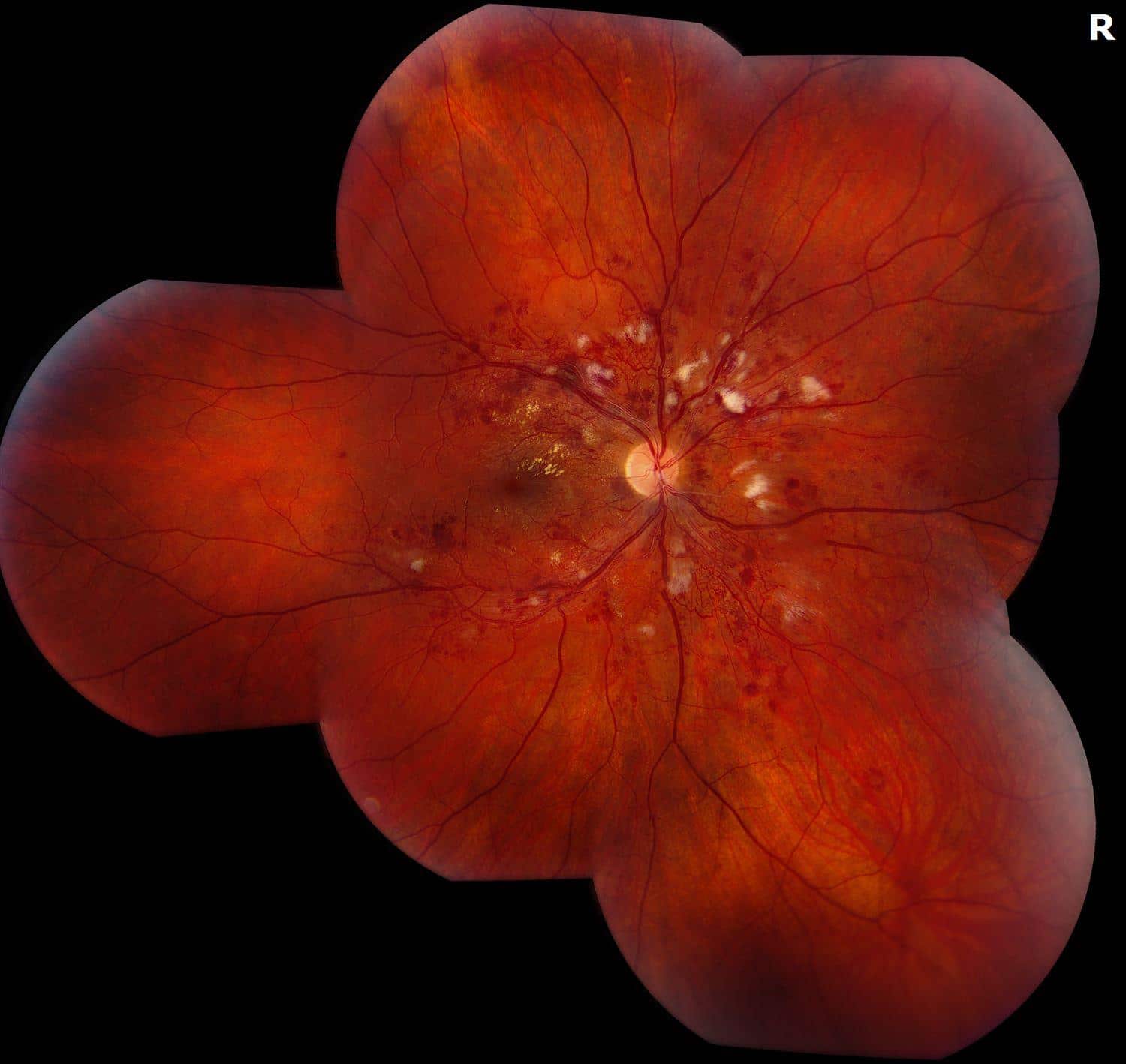
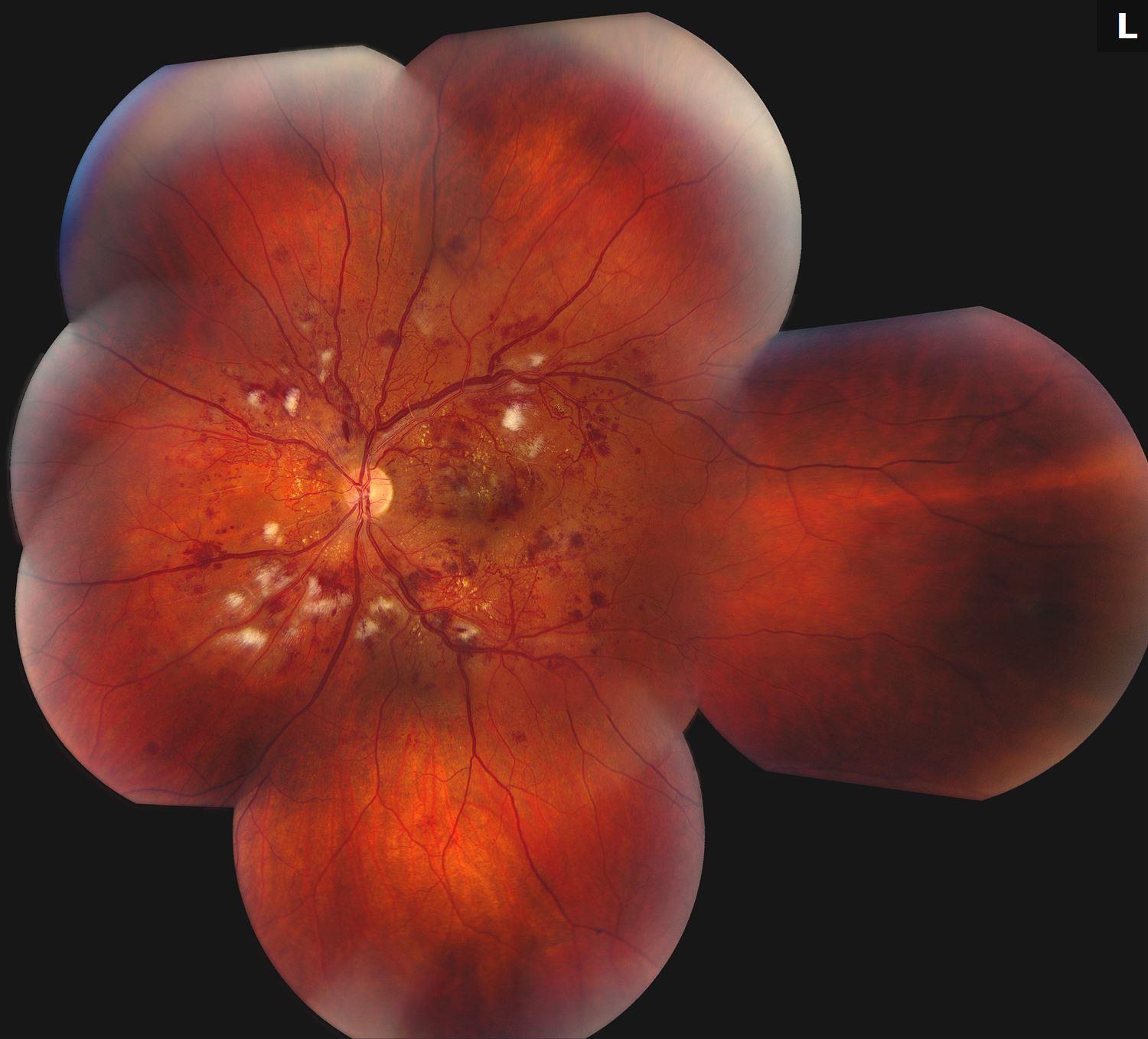
Figure 1. Fundus Photo: The color montage fundus photo of the both eyes show scattered intraretinal hemorrhages encroaching the fovea with flame-shaped hemorrhages along both arcades. Analysis of the vessels shows engorged venules and vessel tortuosity. The periphery of both eyes have multiple dot-blot and flame hemorrhages along both arcades.
OCTs were obtained to further elucidate macular pathology.
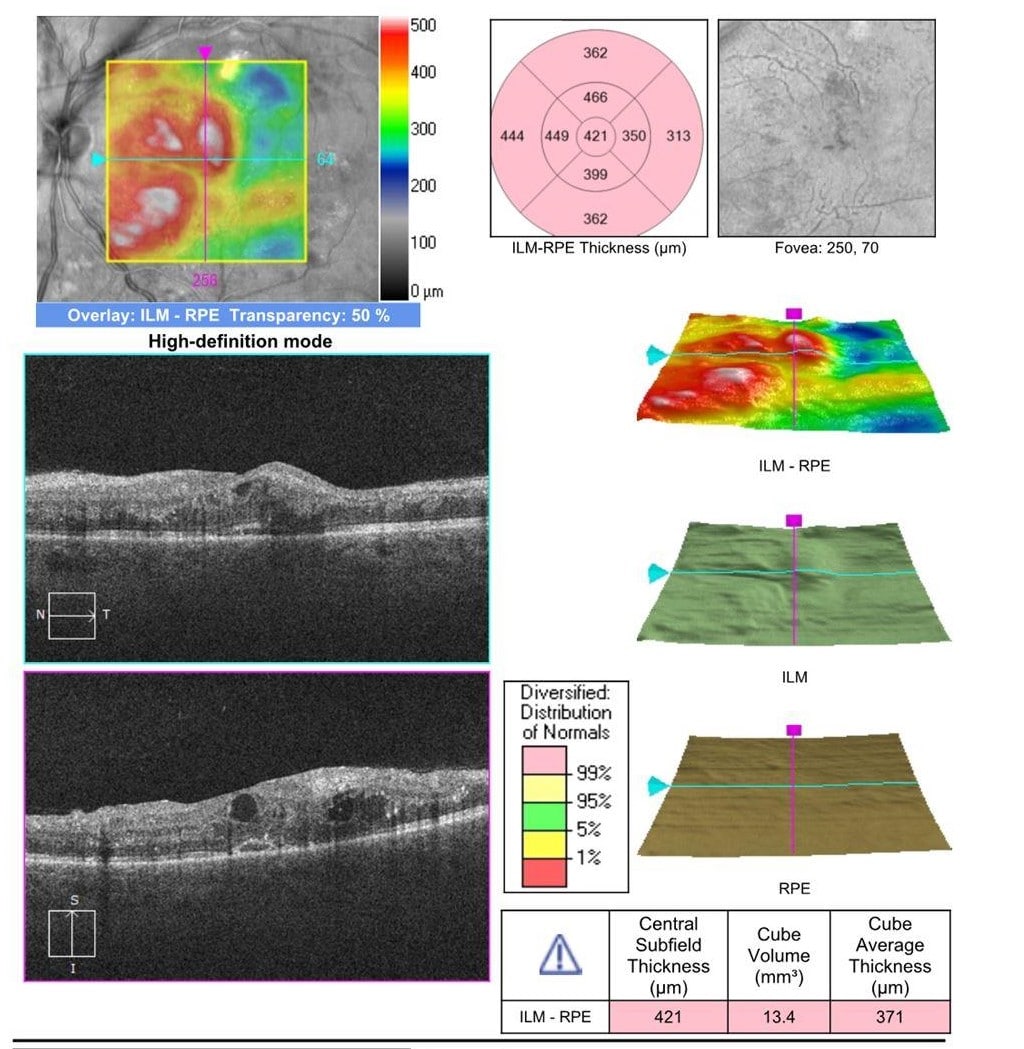
Figure 2. OCT of both eyes shows marked cystoid macular edema with intraretinal hyperreflective material consistent with hard exudates. The left eye OCT also shows some spillover sub retinal fluid.
Finally, a fluorescein angiogram was performed in the office:
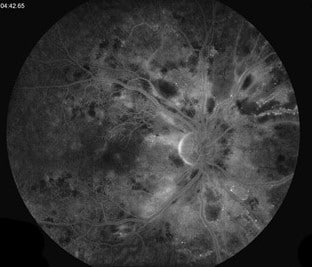
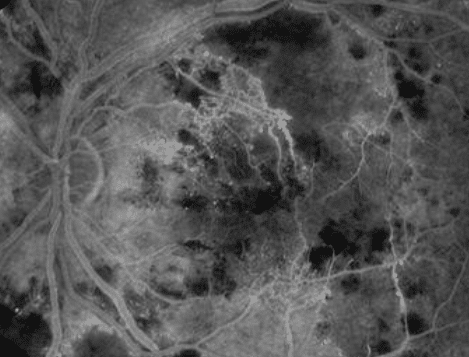
Figure 3. Fluorescein Angiogram of the both eyes showing prominent leakage in the perifoveal area. There was blocking corresponding to the intraretinal hemorrhages. There was decreased perfusion and capillary remodeling of the fovea and macula consistent with an ischemia secondary to his hypertension.
Clinical Course
Given the patient’s extremely elevated blood pressure, he was diagnosed with hypertensive retinopathy with a component of retinal venous occlusion and macular edema. At that time, intravitreal anti-VEGF injections were recommended in both eyes due to the existence of significant macular edema of both eyes, extensive non-perfusion, and subretinal fluid. He was also encouraged to maintain close follow-up with his primary care physician for optimization of his blood pressure and diabetes.
The patient received a 2mg/0.05 ml injection of Aflibercept (Eylea®) intravitreally in both eyes. He was scheduled for a follow-up appointment and a repeat injection in 4-5 weeks.
The patient was monitored closely every 1-2 months for intravitreal injections in the left eye. Over the course of 6 months, he was given a total of three injections in each eye. His edema resolved in both eyes and his vision improved from 20/60 to 20/25 in the left eye. His recent OCT, FA, and fundus photos are seen below:
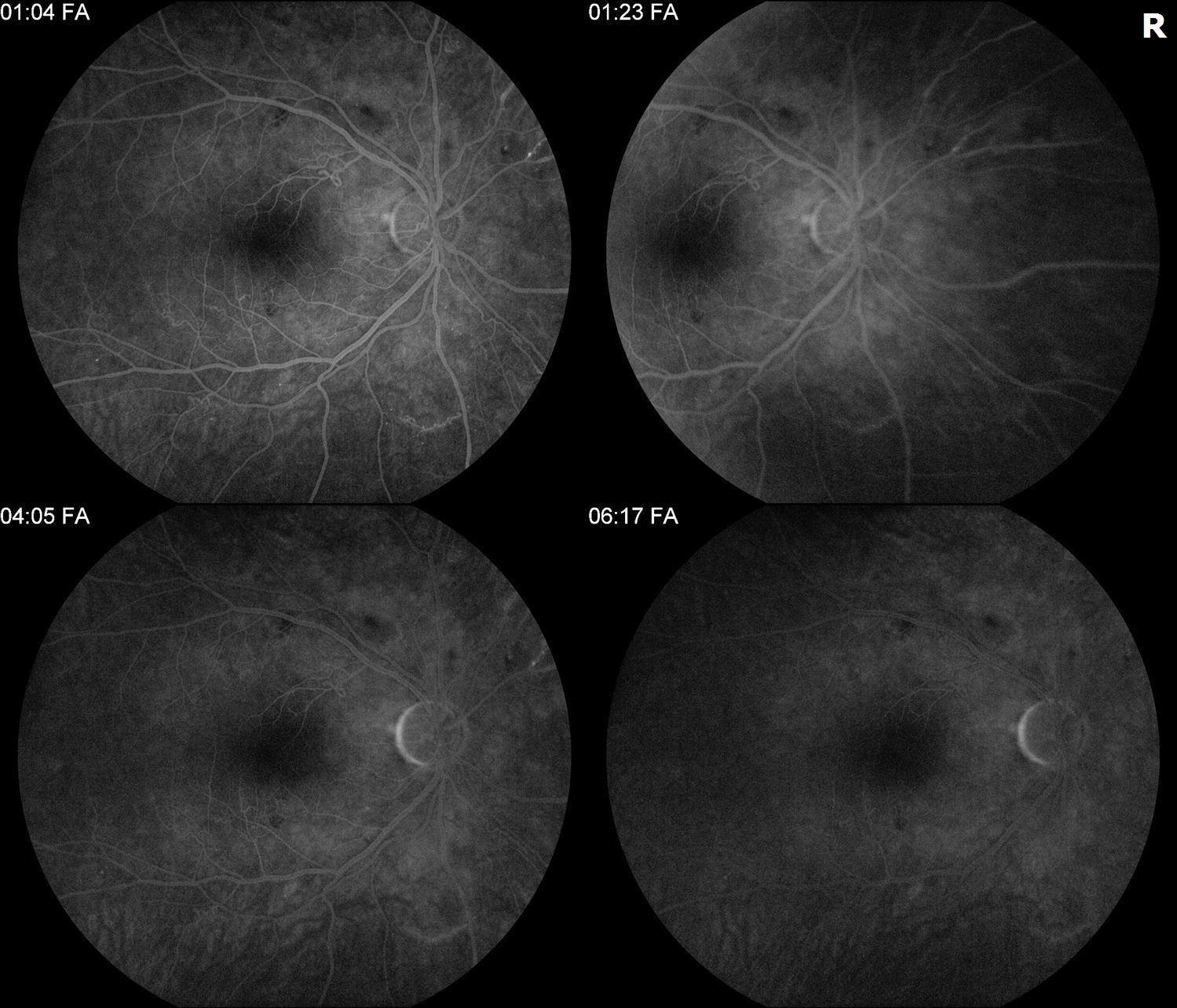
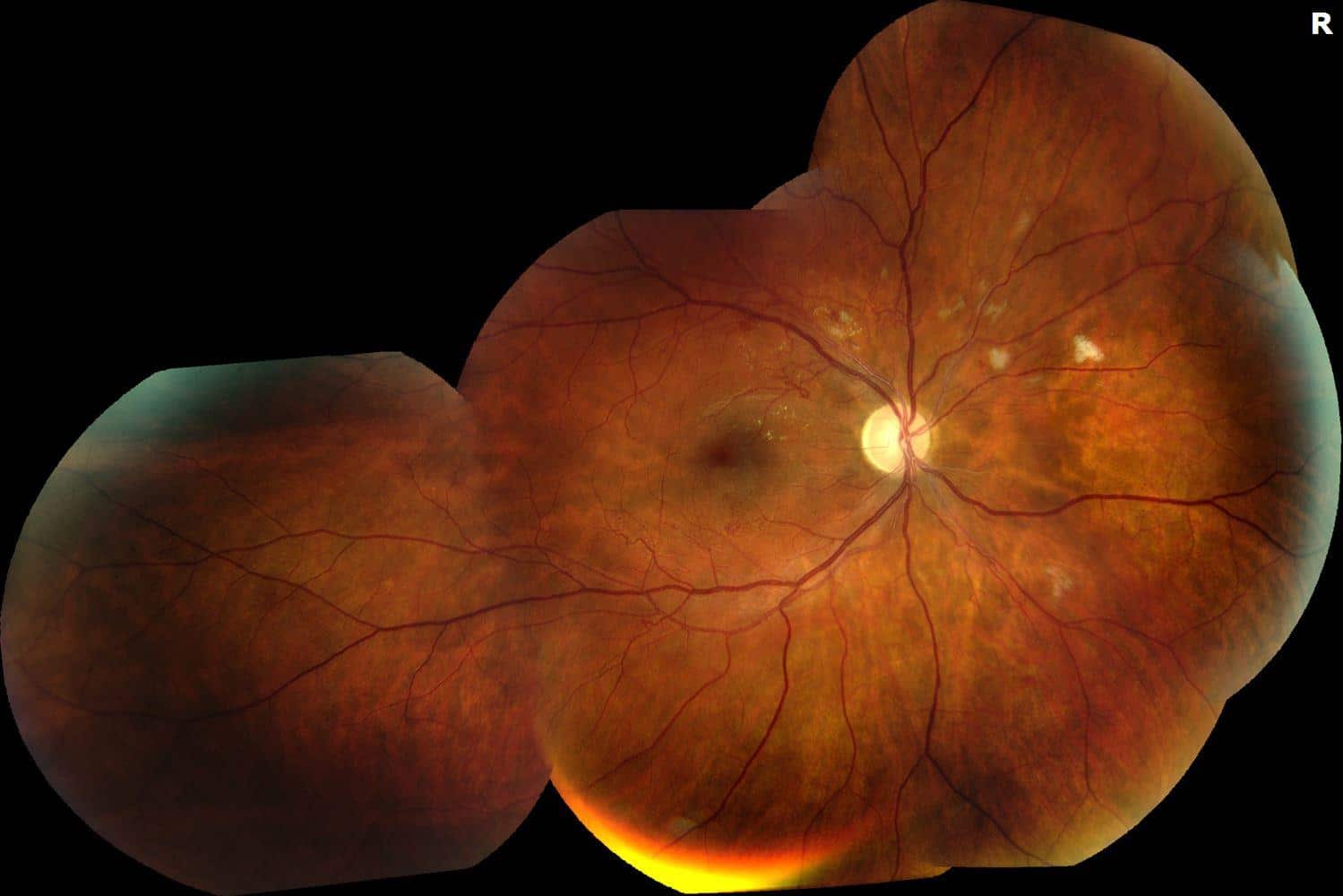
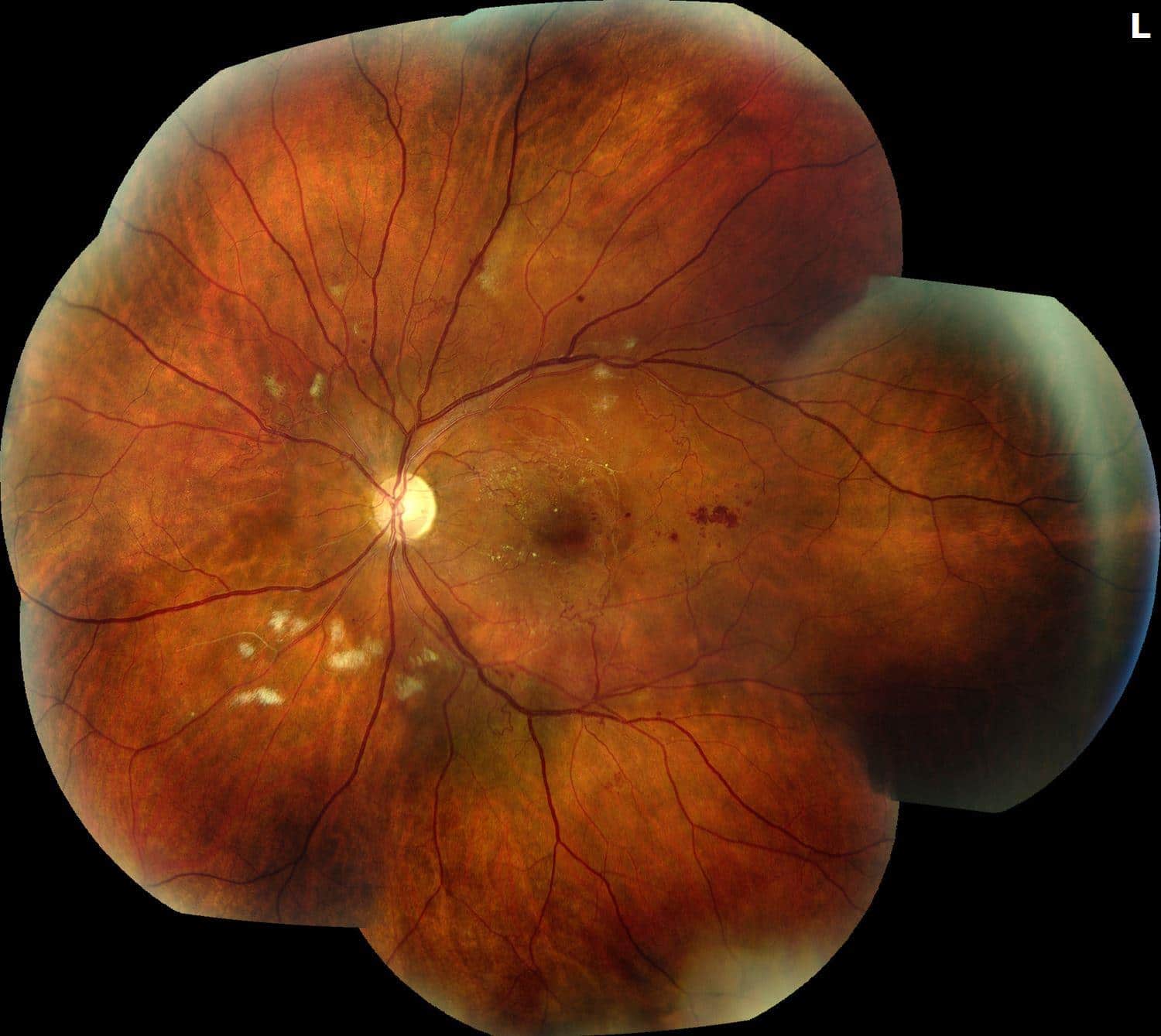
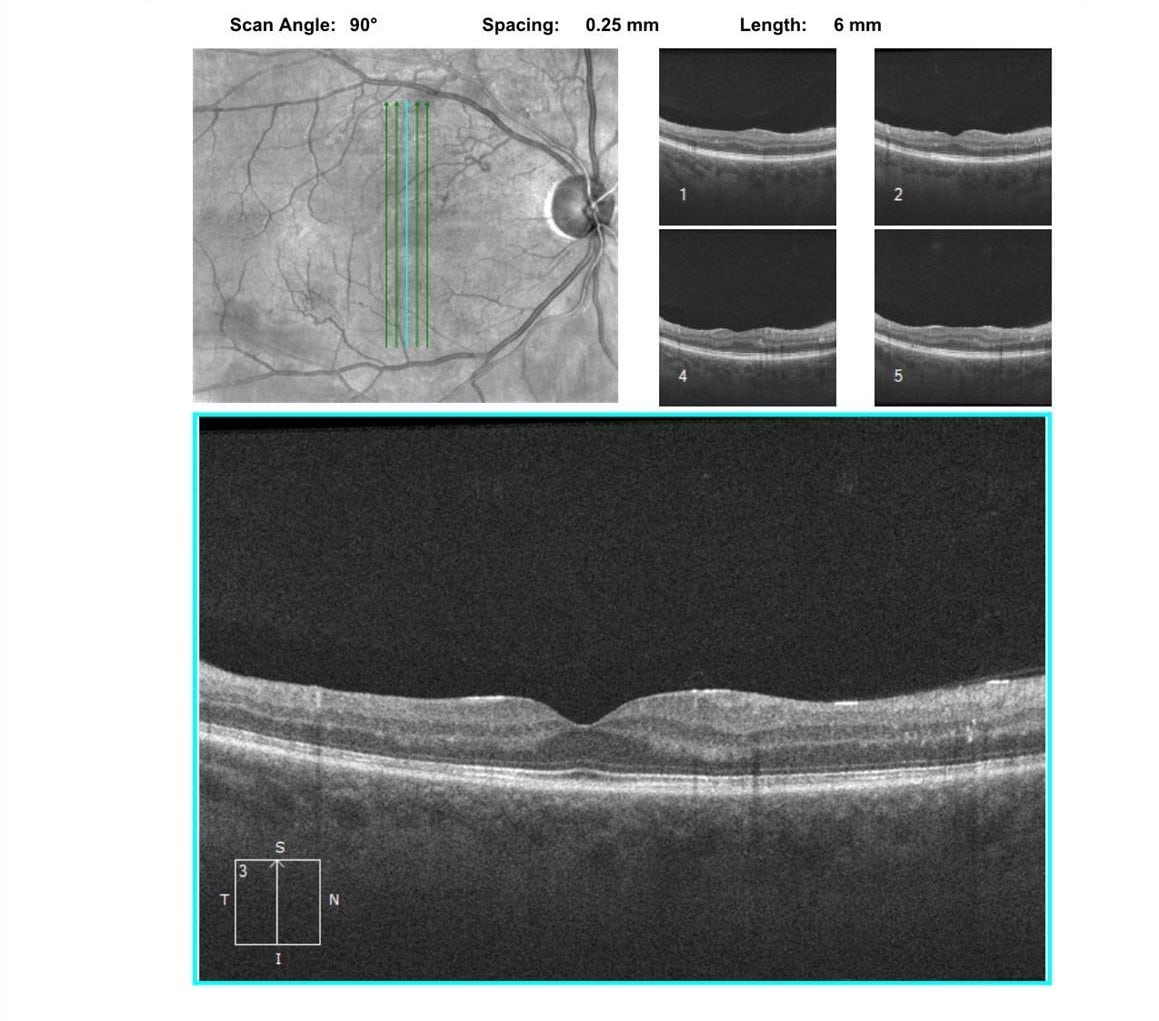
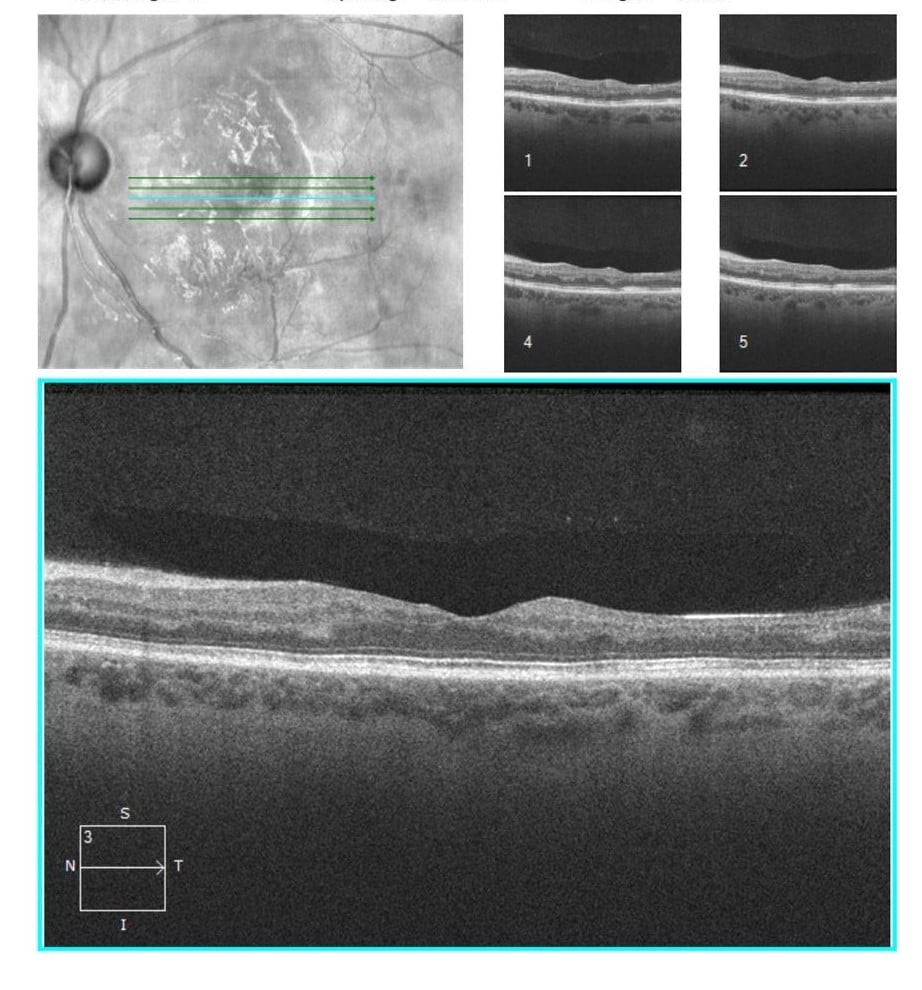
Figure 4. Follow-up FA revealed decreased capillary non perfusion without neovascularization. The OCTs showed resolved edema with some post-occlusive outer retinal atrophy after the series of Aflibercept injections and the fundus photos show improving trace exudates on exam with decreased cotton wool spots and hemorrhages.
Differential Diagnosis:
- Hypertensive Retinopathy
- Bilateral CRVO
- Susac’s disease
- Purtscher retinopathy
- Diabetic retinopathy
- Macular telangiectasia
- Radiation retinopathy
If you are looking to schedule your first consultation, please contact us today by clicking HERE and find the location that is nearest you!

