MEWDS – September 2018

History
A 34 year old man presents with blurry vision in a new “blind spot” in his left eye vision that has been present for ten days. He noticed it has slowly gotten worse. He denies flashes or floaters. His review of systems is otherwise negative except for a recent viral illness four weeks ago that lasted two weeks.
Past medical history: He was recently diagnosed with hypertension and started on Losartan.
Past ocular history: Significant for Lasik OU
Family and social history are unremarkable.
Exam
VA is 20/25+ in the right eye and 20/60+ in the left. IOP was 15 in both eyes.
Anterior segment slit lamp examination is normal bilaterally. The posterior segment of the right eye was normal except for pigment mottling in the macula. The left eye had 1+ vitreous cells and multiple small white spots temporal to the fovea with mild foveal granularity.
Fundus Exam
Left eye reveals white dots in the peripapillary area, the temporal perifoveal area and temporal macula
OCT macula
OD: The right eye is normal with no subretinal fluid or drusen.
OS
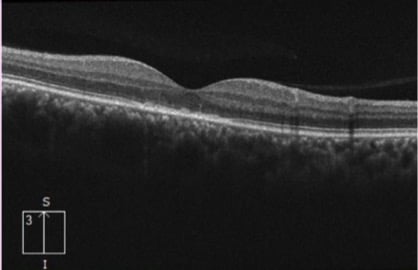
The left eye demonstrates moderate disruption of the ellipsoid layer (IS/OS).
Differential Diagnosis
- Multiple Evanescent White Dot Syndrome (MEWDS)
- Acute Multifocal Placoid Pigment Epitheliopathy (AMPPE)
- Acute Zonal Occult Outer Retinopathy (AZOOR)
- Acute Macular Neuroretinopathy
- Central Serous Retinopathy
- Syphilis
- Idiopathic choroidal neovascularization
FA & FAF
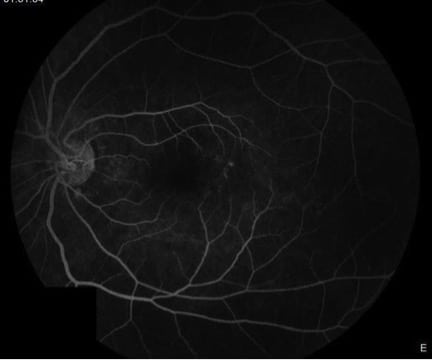
Fluorescein angiogram of the left eye demonstrating hyperfluorescence in the area of the white spots. Some of these spots take on a wreath-like configuration around the nerve.
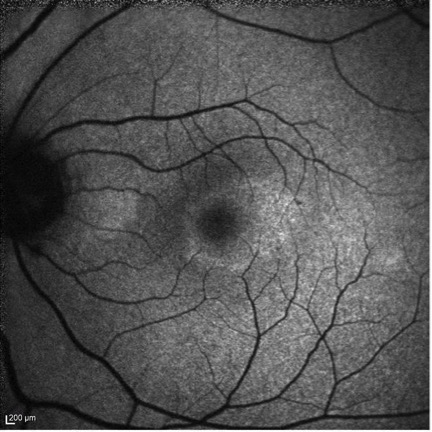
Fundus Autofluorescence of the left eye demonstrating hyperautofluorescense in the area of the white spots clinically.
Diagnosis
MEWDS
Multiple evanescent white dot syndrome is a condition that generally affects younger myopic patients, predominantly women. It is typically unilateral and associated with a viral prodrome. Patients usually report new onset scotoma, sometimes with photopsias. On exam it is characterized by numerous small white dots in the posterior pole. There is often foveal granularity and disc edema as well. Vitreous cells can also be present. OCT often shows disruption of the outer retina, especially the ellipsoid layer. The fluorescein angiogram typically shows “wreath” like patterns in the areas of the white dots. There is often hypocyanescence in these areas on Indocyanine green angiography. Typically the prognosis is favorable with patients improving in 3-10 weeks without treatment.
References
-
Mirza, R., & Jampol, L. M. (2018). White Spot Syndromes and Related Diseases. In Ryan's Retina(6th ed., Vol. 2). Elsevier.
-
Jampol, Lee M. “Multiple Evanescent White Dot Syndrome: I. Clinical Findings.” Archives of Ophthalmology 102, no. 5 (May 1, 1984): 671.

