Retinal Cavernous Hemangioma – July 2020

History
A 10-year-old Caucasian female presented to clinic with referral for abnormal exam findings after she was struck in the face with a tennis ball three weeks prior. She denied any visual complaints. She had no eye pain, no redness, no floaters, no curtain, no veil, and no recent trauma. Her medical history was unremarkable and family history was only significant for migraines in her mother. Review of systems was negative for chest pain, dyspnea, nausea, vomiting, diarrhea, constipation, rashes, or any other systemic symptoms. She denied smoking, alcohol use, or any illicit drug use.
Exam
On exam, her vision was 20/20 in both eyes and IOP was 16 in both eyes. Confrontation visual fields were full bilaterally. Anterior exam was unremarkable. Evaluation of her posterior segment demonstrated clear vitreous bilaterally. Below are her fundus photos:
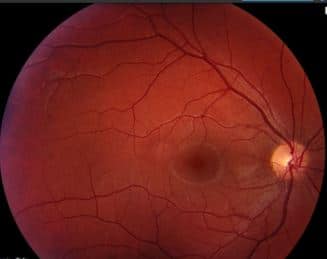
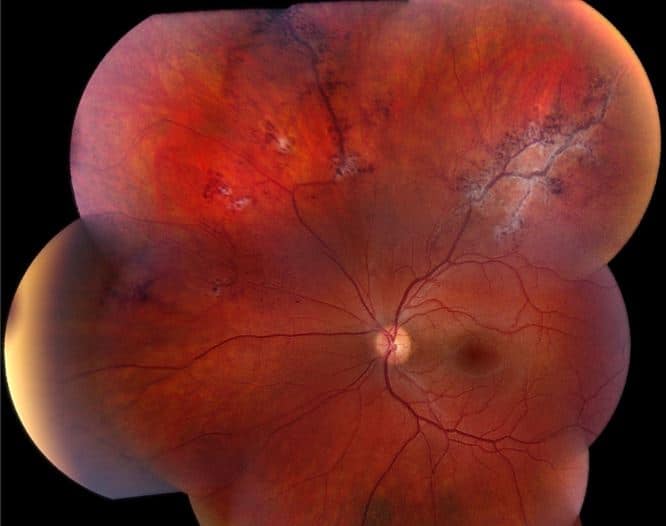
Fundus Photos: Both eyes show pink, healthy appearing nerves with small C:D ratios. The left eye demonstrates superior peripheral retinal areas of intraretinal aneurysms in clumps. There is an overlying area of fibroglial material around the superior lesion at 12 o’clock. There is also peripheral retinal venous dilation. The right eye was unremarkable.
Differential Diagnosis:
- Coat’s Disease
- Leber’s Miliary Aneurysms
- Retinal Cavernous Hemangioma
- Retinal Capillary Hemangioma
- Von Hippel Lindau Syndrome
Discussion:
Retinal Cavernous Hemangioma
Retinal cavernous hemangiomas are benign, vascular hamartomas that are usually asymptomatic and found incidentally. They are normally sporadic in nature, but can occur in an autosomal dominant pattern. They are often unilateral, more common in females (3:2) and classically present as retinal lesions in a “cluster of grapes” like pattern. The appearance is due to dilated vascular sacs in the inner retinal layers without changes in the adjacent arterioles. Histopathologic analysis reveals sessile tumors with thin-walled channels consisting of surface gliosis and non-fenestrated endothelium.
Although usually asymptomatic, retinal cavernous hemangiomas have been reported to cause visual disturbances when they are located in the macula or when macular fibrosis or epiretinal membranes form. They also have rarely been reported to bleed. If analyzed via fluorescein angiography (FA), the lesions show slow filling of the sac-like areas and late staining of the lesions. There is no leakage on FA. Most retinal cavernous hemangiomas can be followed without treatment and with serial exams.
When this lesion is seen on exam, it is important to remember that although benign, it can be associated with systemic findings. Skin and central nervous system hemangiomas may co-exist so the patient should be asked about skin lesions and should have a proper skin exam. Additionally, central nervous system lesions may exist and can lead to complications including intracranial hemorrhages, seizures, and even potentially lead to death. Thus, any patient with a retinal cavernous hemangioma should receive neuroimaging, usually consisting of an MRI of the brain and orbits.
Our patient has done well since diagnosis. MRI brain and orbits with and without contrast revealed cavernous malformations in the left amygdala as well as the left cerebellum. She has been followed now for several years without any acute issues and has maintained excellent vision. She will continue to be followed with serial exams.
If you are looking to schedule your first consultation, please contact us today by clicking HERE and find the location that is nearest you!
References:
- Colvard DM, Robertson DM, Traytmann JC. Cavernous hemangioma of the retina. Arch Ophthalmol 1978;96:2042-4
- Gass JD, Braunste in R. Sessile and exophytic capillary angiomas of the juxtapapillary retina and optic nerve head. Arch Ophthalmol. 1980;98: 1790-1797.
- Siegel AM. Familial cavernous angioma: an unknown, known disease. Acta Neurol Scand 1998;98:369-371
