Toxoplasmosis Chorioretinitis – August, 2020

History
A 31-year-old Caucasian female presented to clinic with intermittent floaters and blurry vision in the right eye for six years. The eye sometimes hurts as well. She had never had any trauma nor eye surgery to this eye. Her medical history was significant only for kidney stones. She did have a family history of glaucoma. Review of systems was negative for chest pain, dyspnea, nausea, vomiting, diarrhea, constipation, rashes, or any other systemic symptoms. She denied smoking, alcohol use, or any illicit drug use.
Exam
On exam, her vision was 20/25 in both eyes and IOP was 16 in the right eye and 20 in the left eye. Confrontation visual fields were full bilaterally. Anterior exam was unremarkable. Evaluation of her posterior segment demonstrated clear anterior vitreous bilaterally without any cells. Below is her fundus photo:
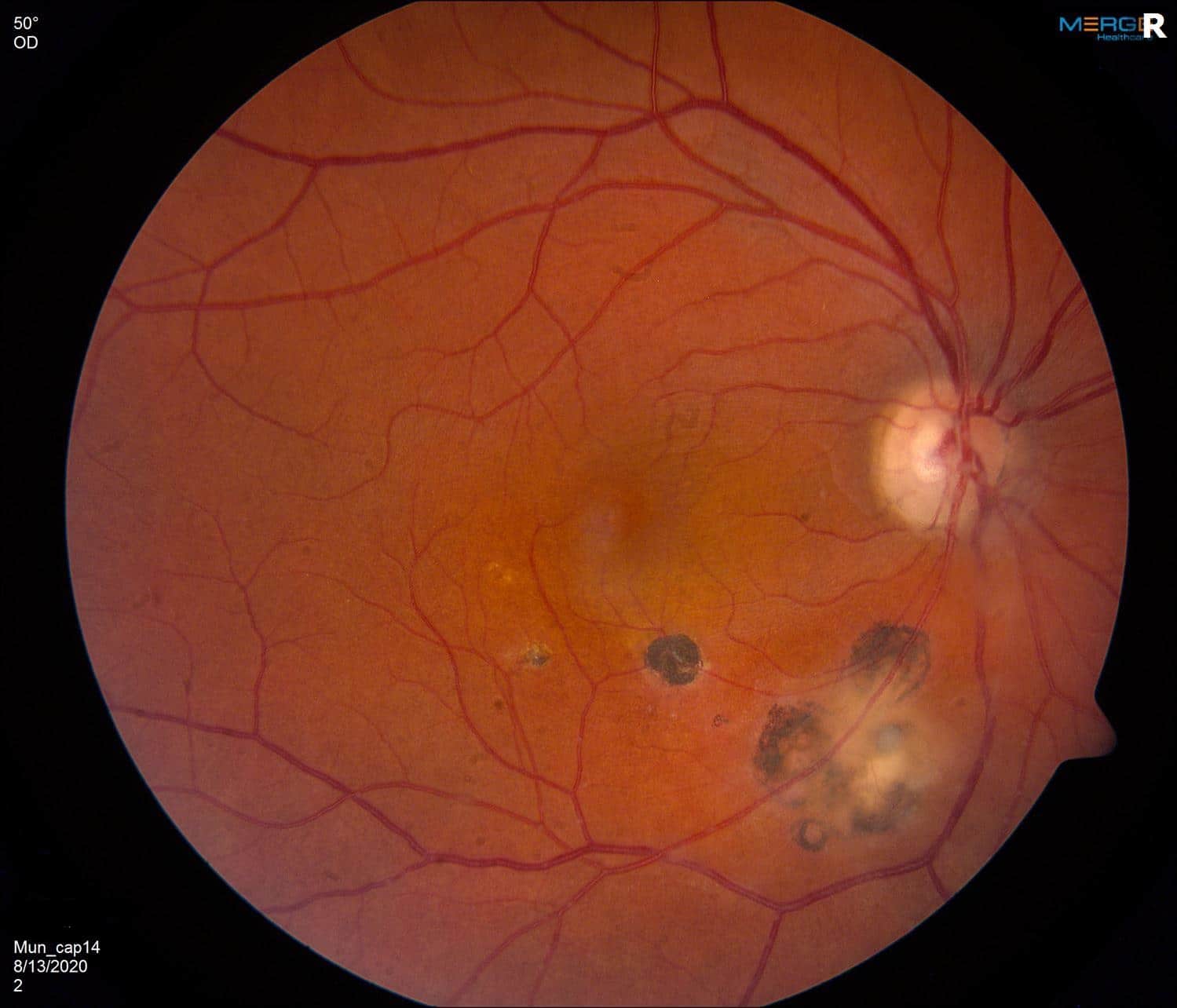
Fundus Photos: The right eye shows a healthy appearing nerve with small C:D ratios. The vessels are within normal limits without perivascular sheathing. There is some scarring along the inferior arcade extending to just inferior to the fovea. There appears to be a fluffy collection in the vitreous overlying some of this scarring. The left eye was unremarkable.
An OCT was obtained and is below:
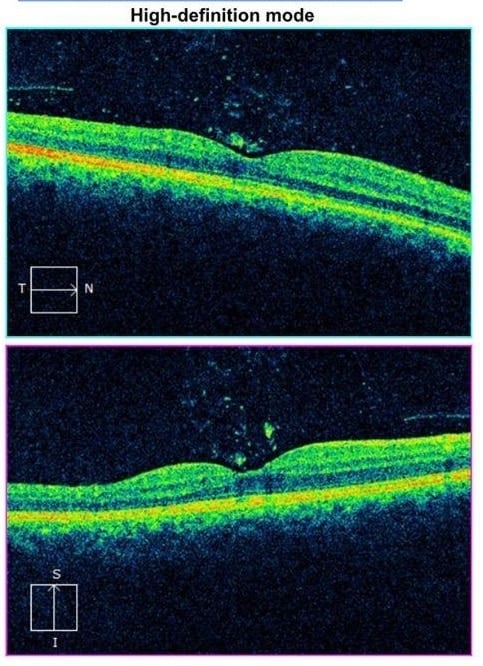
The OCT macula of the right eye demonstrates vitreous opacities consistent with inflammatory cells and a mild vitreomacular adhesion. The OCT is otherwise normal aside from shadowing artifact causing hyporeflectivity in the macula under the vitrous opacities.
Differential Diagnosis:
- Toxoplasmosis chorioretinitis
- Tuberculosis
- HIV Retinitis
- Toxocariasis
- Sarcoidosis
- Syphilis
- Cytomegalovirus retinitis
- Candida endophthalmitis
- Multifocal choroiditis
- Presumed Ocular Histoplasmosis (POHS)
Discussion:
Toxoplasmosis Chorioretinitis
Toxoplasma gondii is a parasitic organism that is globally the most common cause of uveitis of the back of the eye. The parasitic infection is associated with felines such as domestic cats and poorly cooked meat. The bugs could be inactive in the body for years and ultimately reactivate during periods of stress or immunosuppression to result in recurrences.
The resulting, toxoplasma infection can create a chorioretinitis and uveitis in affected individuals. Our patient’s “fluffy” yellow-white vitreous opacity overlying a retinal scar that has indistinct margins is classic for the focal, necrotizing chorioretinitis lesions typical for this disease. It is termed the “headlight in the fog.” Inflammation in the back or even just in the front of the eye may last weeks to months and often improves on its own in patients with intact immune systems.
As a result, lesions that are not near the macula or center of vision are frequently managed with observation. Retinologists are particularly careful with pregnant patients to avoid undue side effects to the unborn child. In those with vision-threatening infections, treatment may include an intravitreal injection of clindamycin, oral antibiotics, and/or topical anti-inflammatory drops. One to two days after commencement of these interventions, high dose oral prednisone is often utilized. Intraocular steroids are avoided so as to prevent spreading of the infectious retinitis.
Methods for preventing toxoplasma chorioretinitis include hand washing, cooking meat well, and wearing gloves to clean cats’ litter boxes. Patients who have weakened immune systems or women at risk of or already pregnant should avoid contact with cats and under cooked meats.
If you are looking to schedule your first consultation, please contact us today by clicking HERE and find the location that is nearest you!
References:
- Desmonts G, Couvreur J. Congenital toxoplasmosis: A prospective study of 378 pregnancies. N Engl J Med 1974; 290(20):1110-6.
- Bonfioli AA, Orefice F. Toxoplasmosis. Seminars in Ophthalmology. 2005;20:129-41.
- Tabbara KF and O’Connor GR. Treatment of ocular toxoplasmosis with clindamycin and silfadiazine. Ophthalmology 1980;87:129-34.

