Astrocytic Hamartoma – November 2018

History:
The patient is a 10 year old boy who was referred for a stable mass in the posterior pole. The patient was first seen by the referring provider 3 years ago as a routine school evaluation and the lesion has not changed since then. He has no other medical history.
He denies any vision disturbances or double vision. His parents have not noticed any history of eye turning.
Exam:
On exam his visual acuity is 20/25 OU and his IOP is 15 and 16. He is orthophoric and demonstrates full extraocular movements.
On slit lamp exam, his eyes are white and quiet with a normal cornea, anterior chamber, iris and lens in both eyes. He does not have anterior chamber or vitreous cells in either eye.
His fundus exam of the right eye is normal. In the left eye there is a white, somewhat translucent, elevated lesion, roughy 1 DD in diameter, adjacent to the nerve along the inferotemporal arcade.
Fundus photo of the left eye demonstrating the lesion.
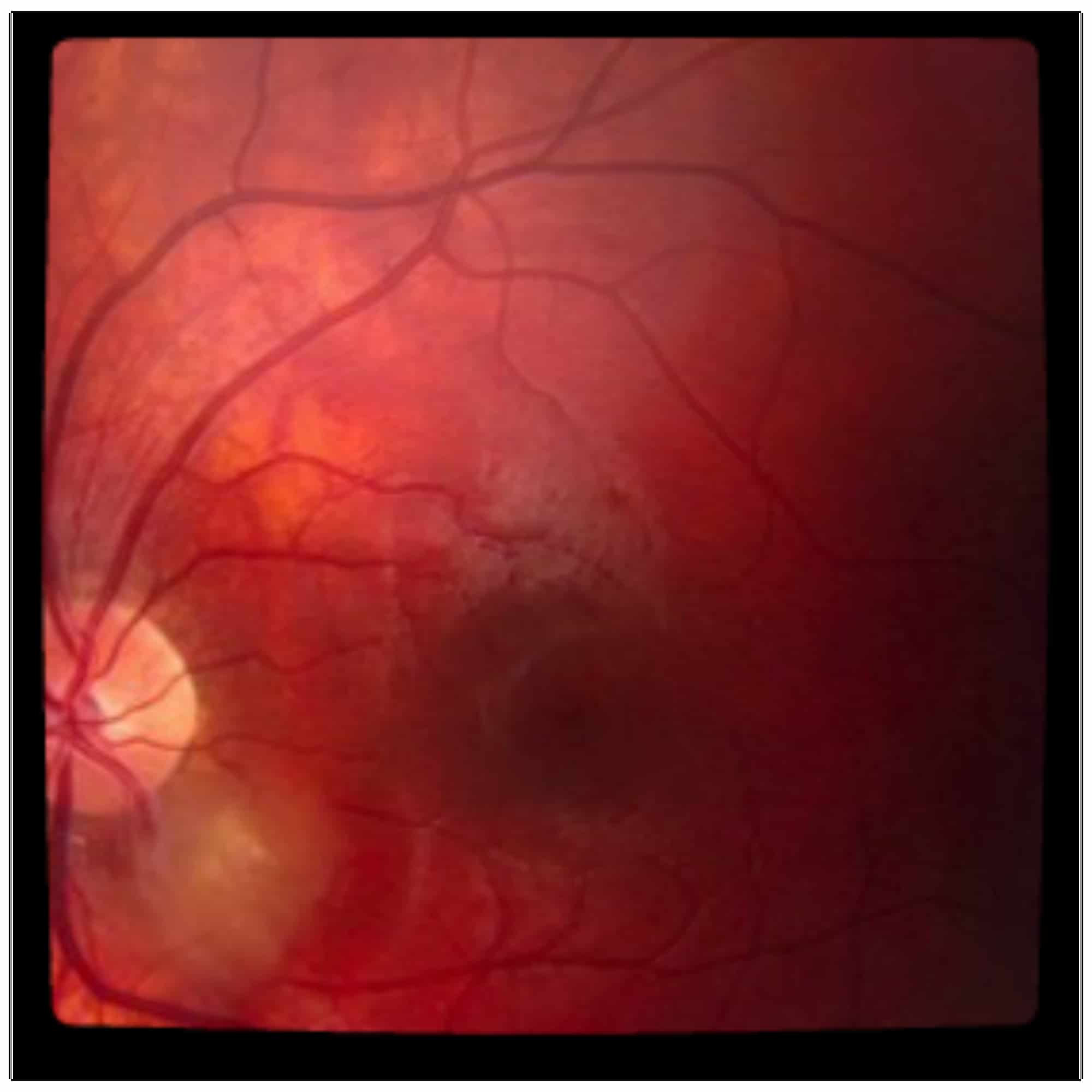
Differential Diagnosis
- Retinoblastoma
- Retinocytoma
- Astrocytic Hamartoma
- Osteoma
- Toxocara granuloma
- Sarcoidosis
- Infectious Chorioretinitis
- Syphilis
- Tuberculosis
OCT
The OCT demonstrates that the lesion originates from the nerve fiber layer. There are also optically empty spaces and shadowing within the lesion.
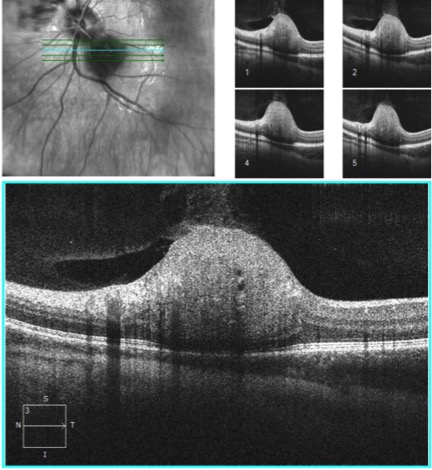
B-Scan
B- scan ultrasound demonstrates a 1.36 mm lesion with high internal reflectivity.
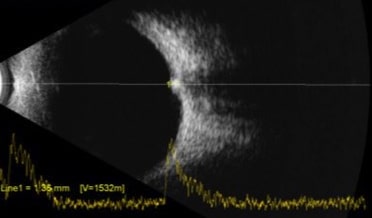
Given the findings of a non-progressive, elevated, vascularized lesion within the inner retina, whith high internal reflectivity on B-scan ultrasound, the diagnosis of Astrocytic Hamartoma was made.
Diagnosis: Astrocytic Hamartomas (Astrocytoma)
These gliomas present as nodular masses at or near the optic disc. They are typically white and can be opaque or translucent and are often calcified. Occasionally they present as flat smooth tumors. They grow in the Nerve fiber in an endophytic pattern (in toward the vitreous cavity), though there are rare cases of exophytic growth leading to retinal detachment. They generally show minimal or no growth, and occasionally regress on their own. Their nodular nature gives them the classic “mulberry” appearance.
These tumors have varying degrees of vascularization and on fluorescein angiogram they typically demonstrate late-phase hypefluorescence with leakage in to the vitreous. On OCT these lesions are seen to originate from the nerve fiber layer, and they typically show optically empty spaces.
Complications of astrocytic hamartomas include vitreous hemorrhage, thought to be due to the vascular proliferation within the lesion, and the occasional development of a choroidal neovascular membrane at the edge of the lesion.
There are important considerations when identifying a astrocytic hamartoma. The first is that these lesions must be differentiated from retinoblastoma, which can be difficult as both lesions typically present with calcified masses of the retina in young children, though retinoblastoma demonstrates growth.
It is also important that the patient undergo workup for tuberous sclerosis and neurofibromatosis as these are the most common systemic associations of astrocytic hamartomas. Tuberous sclerosis can be identified by the classic triad of seizures, facial angiogibromas, and developmental disability, although this triad only occurs in around 30% of cases. These patients tend to develop astrocytic hamartomas in childhood and the lesions are often bilateral or multifocal. MRI or CT scan can be useful to identify lesions in the brain.
References:
-
Cruess A.F., & Sharma, S. (2018). Tuberous Sclerosis and the Eye. In Ryan’s Retina(6th ed., Vol. 2). Elsevier.
-
Shields CL, Say EA, Fuller T, et al. Retinal astrocytic hamartoma arises in nerve fiber layer and shows “moth-eaten” optically empty spaces on optical coherence tomography. Ophthalmology. 2016;123:1809–1816

