Best Vitelliform Macular Dystrophy – October, 2022

History:
A 32-year-old female presented with complaints of decreased vision in both eyes for 6 months. She endorsed some pressure sensation in both eyes but denies flashing lights, floaters, curtains over vision. She had a past medical history for depression, controlled on Lexapro. Her review of symptoms is noncontributory.
Exam:
Her visual acuity was 20/20 in both eyes. Her pupils were normally reactive without RAPD. Her intraocular pressure was 16 in both eyes. Anterior segment exam was significant for mild punctate epithelial erosions in both eyes. Her dilated exam showed multiple vitelliform lesions with retinal pigment epithelial changes in the macula in both eyes. There were no hemorrhages, exudates, or edema noted. The peripheral exam was normal.
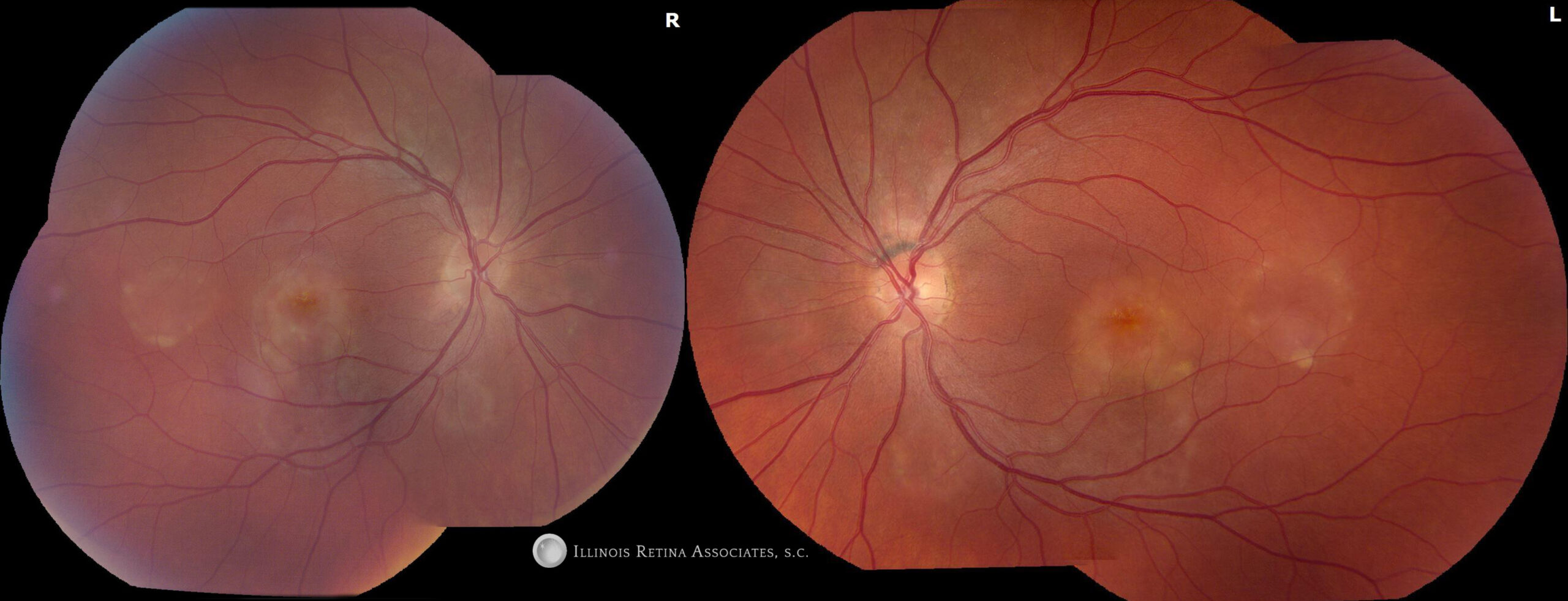
Figure 1: Fundus photography showed hypopigmentation in the posterior pole. There were noted to be round, deep retinal hypopigmentation in the macula and just beyond the arcades. Of note, changes are very symmetric.
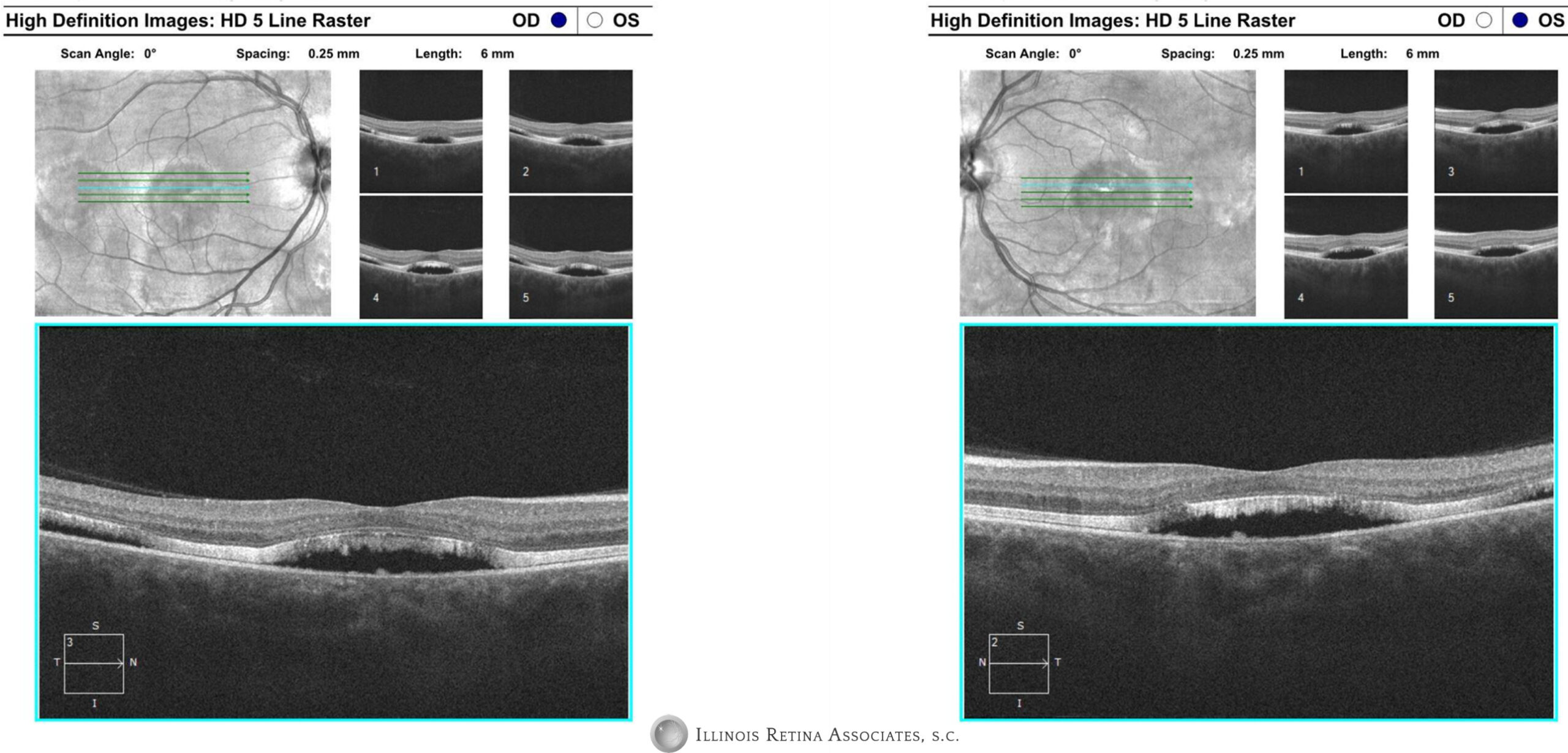
Figure 2: Optical coherence tomography (OCT) of the macula showed symmetric subfoveal subretinal fluid in both eyes with very mild intraretinal cystic changes. There was also mild subretinal fluid temporal to the macula in both eyes.
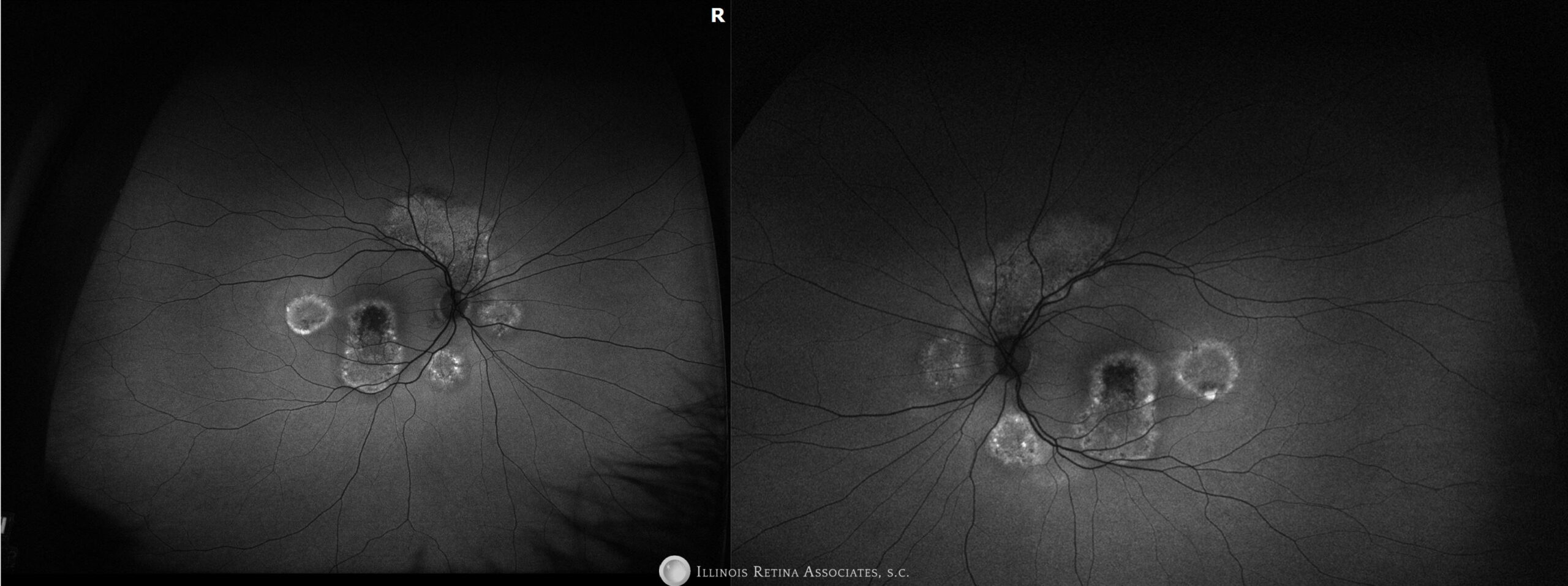
Figure 3: Fundus autofluorescence of both eyes showed well circumscribed areas of hyper- and hypo-autofluorescence in both eyes. There appeared to be a guttering configuration related to the macular lesion in both eyes.
Differential Diagnosis:
- Best vitelliform macular dystrophy
- Central serous chorioretinopathy
- Toxoplasmosis retinopathy
- Autosomal dominant macular drusen
Discussion:
Best Vitelliform Macular Dystrophy
Best vitelliform macular dystrophy, also known as Best disease, is described as a hereditary retinal dystrophy affecting the retinal pigment epithelium which leads to a bilateral yellow “egg-yolk” appearance of the macula. The fundus lesions tend to appear in late childhood to early adulthood. Visual prognosis is relatively good. Classically, Best disease is inherited autosomal dominantly but shows variable penetrance and expressivity. Best disease is caused by a mutation in the bestrophin genes. Bestrophins are transmembrane proteins which are found in highest density in the retinal pigment epithelium in the foveal area. Defects in this gene cause abnormal ion transportation.
Diagnosing Best disease can typically be done clinically but there are classic imaging findings that are consistent with the diagnosis. Electro-oculogram is universally abnormal with an Arden ratio less than 1.5. Electro-retinogram is normal. Fundus autofluorescence tends to highlight more lesions that can be seen on exam or fundus photography.
There are six classic stages to Best disease:
- Stage I, Previtelliform: normal vision, normal or only slightly mottled retinal pigment epithelial changes with an abnormal EOG.
- Stage II, Classic Vitelliform: classic “egg yolk” appearance becomes visible. Vision remains relatively normal but there can be mild vision impairment
- Stage III, Pseudohypopyon: lipofuscin products begin to layer within the lesions.
- Stage IV, Vitelleruptive: appearance resembles “scrambled eggs” due to breakdown of materials collected subretinal. Vision tends to remain good but can start to be affected.
- Stage V, Atrophic: Central retinal pigment epithelial atrophy begins in the affected areas. Vision may range from 20/20 to 20/200 based on the location and size of atrophy.
- Stage VI, Choroidal neovascularization: Affects about 20-25% of patients. Vision can become severely impacted.
There is no specific management of Best disease until there is clinically significant choroidal neovascularization. Anti-VEGF and photodynamic therapy have both been used.
If you are looking to schedule your first consultation, please contact us today by clicking HERE and find the location that is nearest you!
References:
- Johnson AA et al. Bestrophin 1 and Retinal Disease. Prog Retin Eye Res. 2017 May ;58: 45–69. doi:10.1016/j.preteyeres.2017.01.006.
- Marmorstein A.D. et al. Bestrophin, the product of the Best vitelliform macular dystrophy gene (VMD2), localizes to the basolateral plasma membrane of the retinal pigment epithelium. Nat. Acad. Sci. 97: 12758-12763, 2000.
- Schachat A.P., Wilisoson CP., Hinton DR., Sadda SR., Wiedemann P. Ryan’s Retina 6th edition, Elsevier (2018).

