Central Retinal Artery Occlusion With Cilioretinal Artery Sparing – June, 2021

History
A 67-year-old man presented to clinic with complaints of acute vision loss in the right eye. He had no eye pain, no redness, no trauma, no flashes, and no floaters. Review of systems was negative. His medical history was significant for diabetes, hypertension, hyperlipidemia, and coronary artery disease. He had a 20-pack year smoking history, but denied alcohol use or illicit drug use.
Exam
Vision was 20/200 in the right eye and 20/25 in the left eye, respectively. IOP was 14 and 13. There was a right sided relative afferent pupillary defect with sluggish constriction. Confrontation visual fields were significantly constricted OD, but full OS. Anterior exam of the both eyes unremarkable. Evaluation of his posterior segment demonstrated vitreous syneresis OU. Below are his fundus photos:
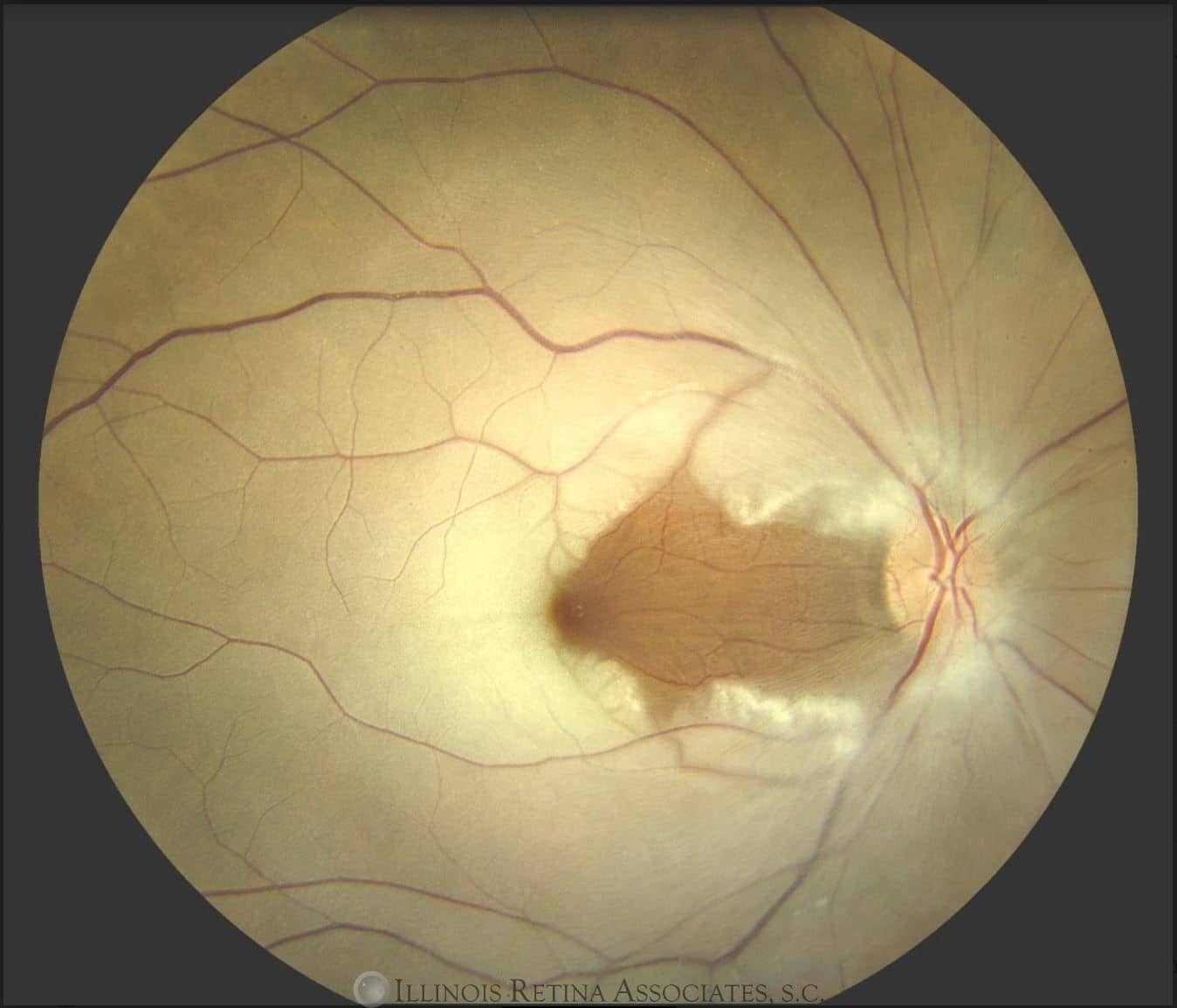
Fundus Photos: Right eye showed a mildly edematous optic nerve with 0.2 C:D ratio. There was diffuse retinal whitening but good retinal perfusion between the nerve and the fovea. Peripheral exam showed diffuse arterial boxcarring and further whitening.
Differential Diagnosis:
- Branch Retinal Artery Occlusion
- Central Retinal Artery Occlusion with cilioretinal artery sparing
- Ophthalmic Artery Occlusion
- Ocular Ischemic Syndrome
- Carbon Monoxide Poisoning
Discussion:
Central Retinal Artery Occlusion with Cilioretinal Artery Sparing
Acute artery occlusions, whether branch or central, should be considered emergent conditions and should prompt emergent referral to the nearest stroke center for evaluation. Patients often present with sudden, painless vision loss over seconds. If seen in the acute setting, examination will reveal retinal whitening, a possible “cherry red spot,” sluggish blood flow, and vascular narrowing. Retinal artery occlusions often lead to very significant vision loss (20/200 or worse), but if presenting with hand motion to NLP vision, they may in fact have an ophthalmic artery occlusion. Occasionally, as in this patient, there can be sparing of a cilio-retinal artery (present in up to 50% of the population), which may help maintain some central vision (even 20/20), but still leads to significant peripheral field loss. Although several therapies have been discussed as possible management steps, including ocular massage, there have been no studies that demonstrated efficacy in improving visual outcomes.
Retinal artery occlusions are often due to blockages of retinal blood flow from an embolus, but can also be due to underlying inflammatory conditions or trauma. Similar to ischemic strokes, CRAO risk factors include smoking, hypertension, diabetes, and cardiovascular disease. Retinal artery occlusions in patients over 50 years old should raise concern for possible giant cell arteritis. After emergent evaluation for possible stroke or GCA is completed, these patients should be followed by ophthalmology as they can develop neovascularization.
Our patient was referred immediately to the emergency room for evaluation. After optimization of risk factors and appropriate management, they will return for follow-up and monitoring for further ophthalmic complications.
If you are looking to schedule your first consultation, please contact us today by clicking HERE and find the location that is nearest you!
References:
- Brown GC,and Shields JA. Cilioretinal arteries and retinal artery occlusion. Arch Ophthalmol 1979;97:84-92
- Hayreh SS, Kolder HE, Weingeist TA. Central retinal artery occlusion and retinal tolerance time. Ophthalmology 1980; 87:75-78
- Rudkin AK, Lee AW, Chen CS. Ocular neovascularization following central retinal artery occlusion: prevalence and timing of onset. Eur J Ophthalmol 2010 May 28 Epub
- Schumacher, M. et al. Central retinal artery occlusion: local intra-arterial fibrinolysis versus conservative treatment, a multicenter randomized trial. Ophthalmology 117,1367–1375.e1 (2010)

