Chorioretinal Colobomas – February, 2022

History
A 41 year-old female patient presented from optometry for a central visual field defect in the left eye. The patient described a slow, progressive loss of vision in the left eye over many years. She had a retinal detachment of the right eye that was repaired many years ago with vitrectomy and scleral buckling. The optometrist’s referral note presented an impressive differential of possible diagnoses (discussed below) related to the abnormalities found on exam.
Past medical history was noncontributory, though she had had nasal surgery 4 years prior for allergic sinusitis. Patient was taking prescription oral contraceptive pills as well as over the counter loratadine.
Exam
The patient’s vision was 20/200 in the right eye and 20/30 in the left eye. Intraocular pressure was 15 and 17 in the right and left eye, respectively.
Her anterior segment was normal, but her posterior segment revealed an abnormal optic nerve in the left eye with a blunted macular reflex. Macular pigmentary changes were present in both eyes.
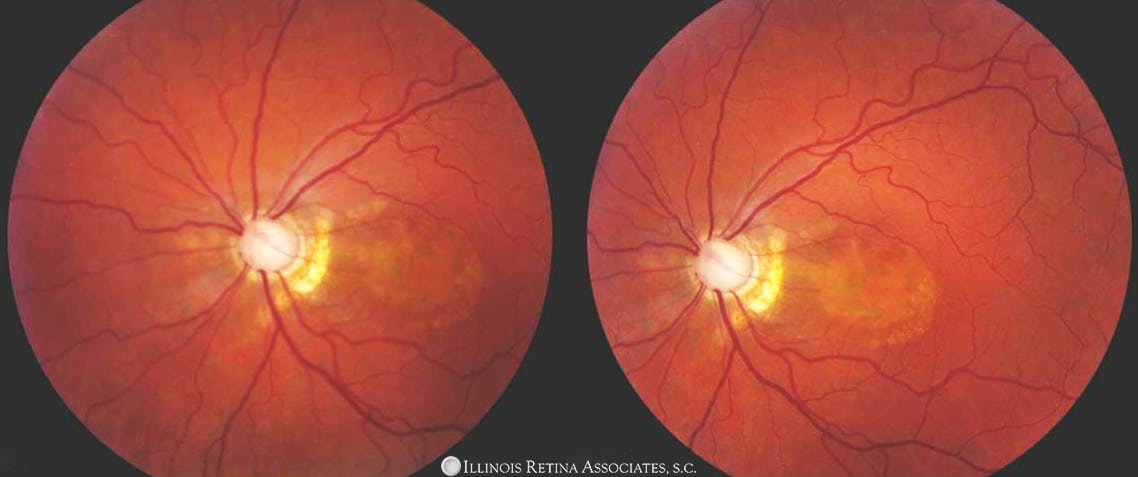
Figure 1. Color fundus photo of the left eye demonstrates a cavernous optic nerve and the aforementioned clinical finds.
A fluorescein angiogram was obtained to further elucidate the nature of these findings.
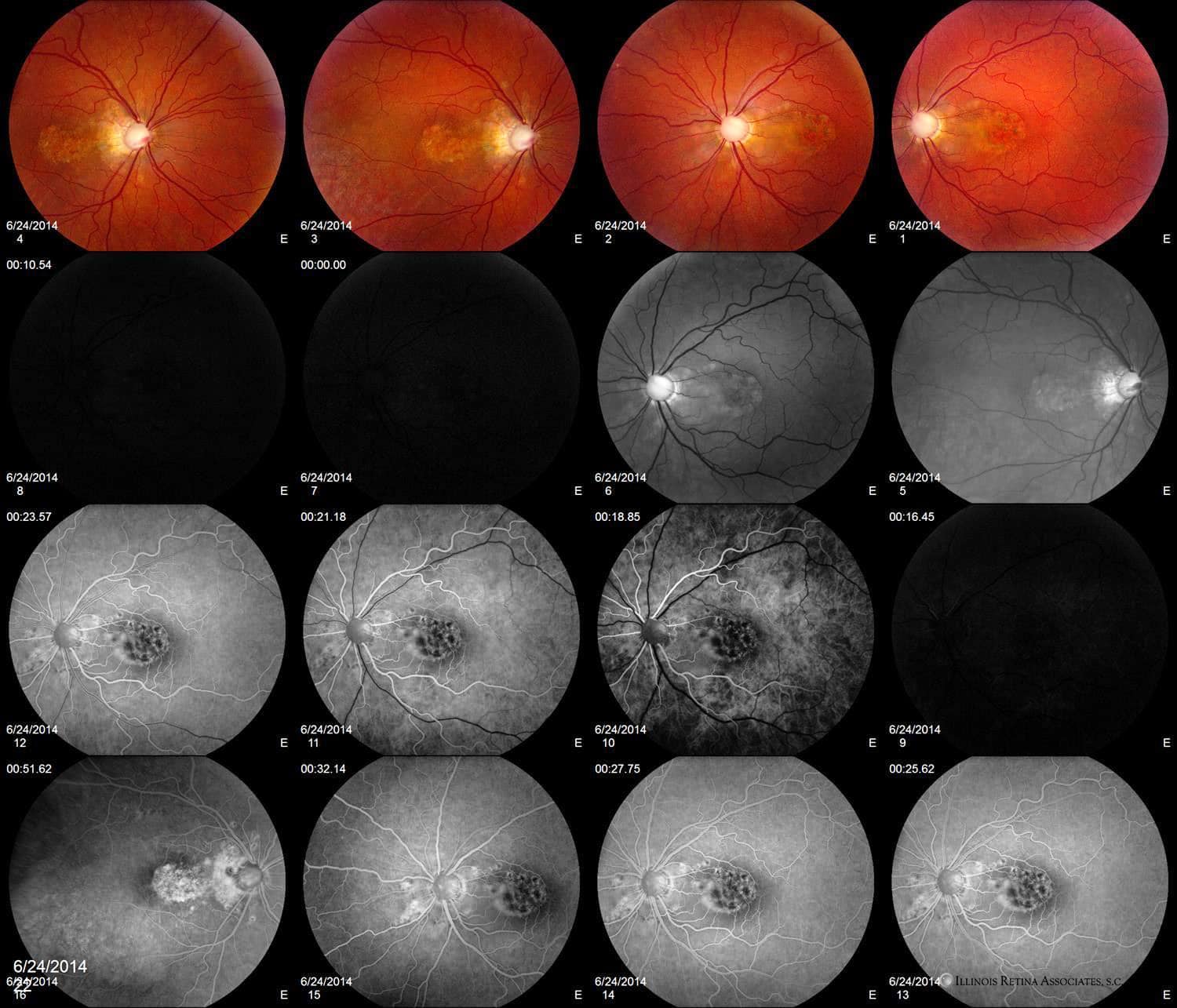
Figure 2. Additional color fundus photos and fluorescein angiogram showing bilateral cavernous optic nerves with early maculo-papular window defects and late variable staining of the parafoveal region.
The optic nerve abnormalities stood out, and additional information was gleaned from OCT imaging.
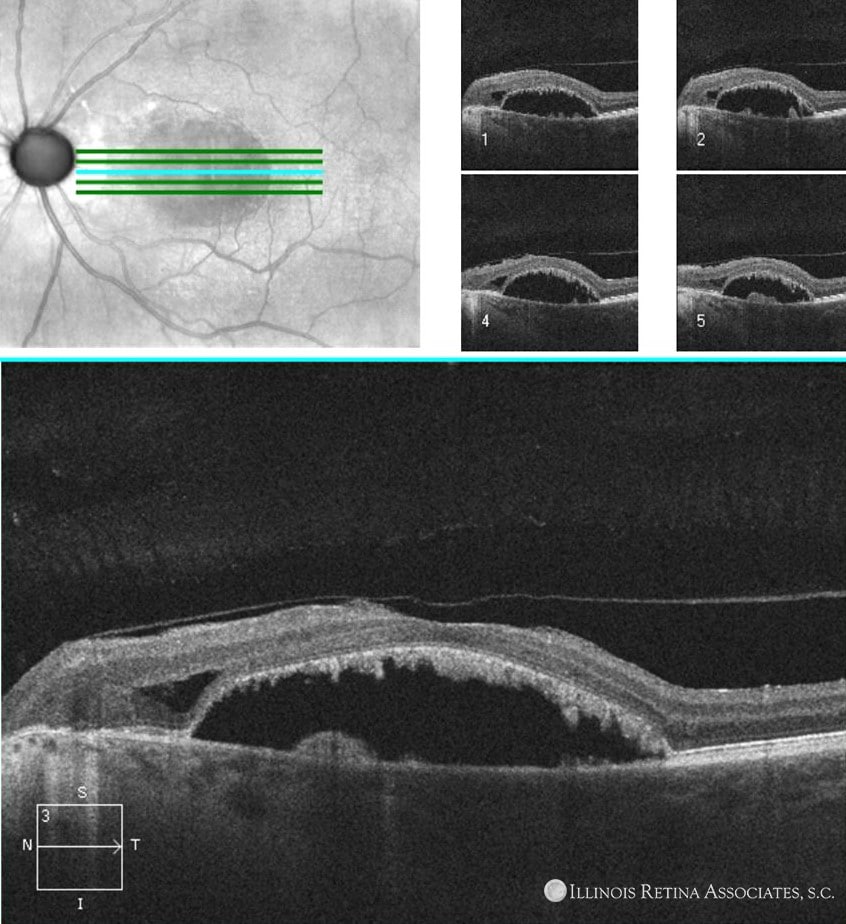
Figure 3. OCT of the macula demonstrates an epiretinal membrane with a schisis cavity and serous retinal detachment involving the fovea. Remarkably, the ellipsoid zone appears robust.
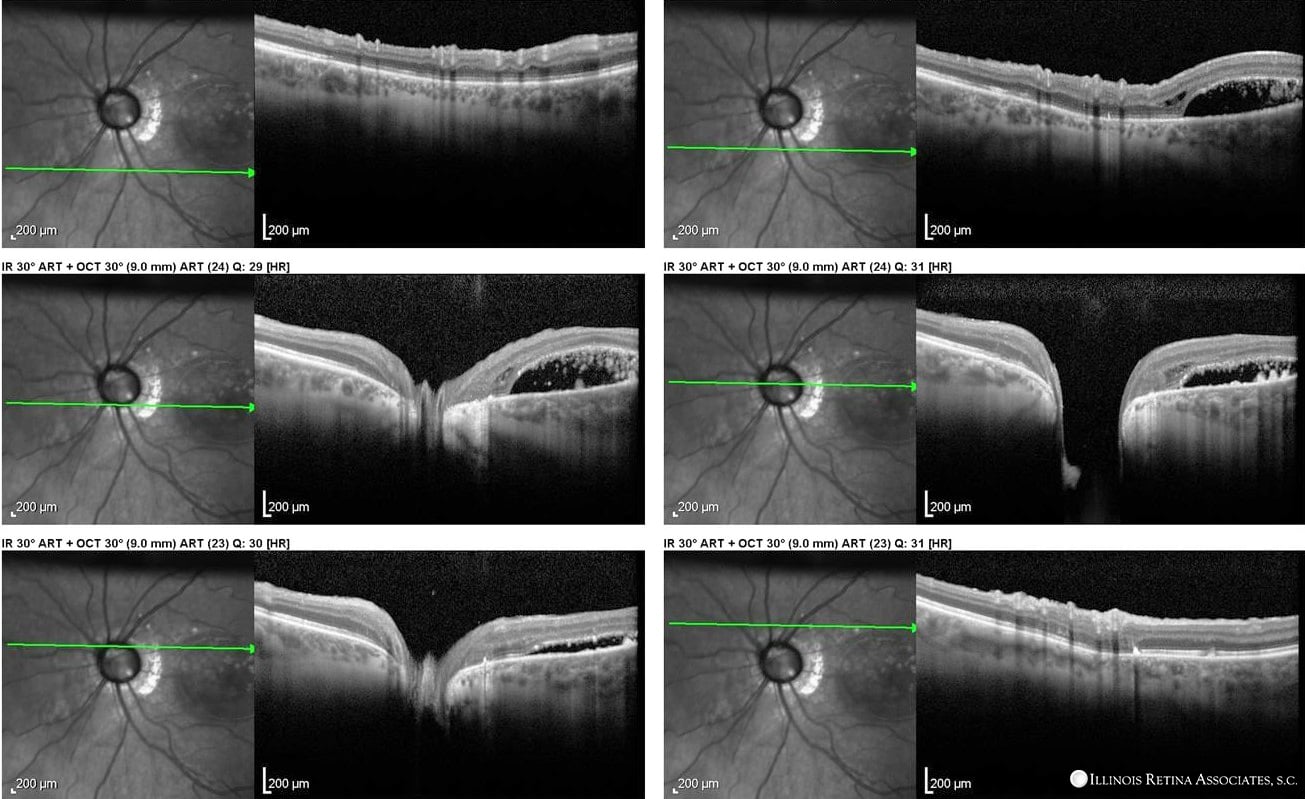
Figure 4. OCT of the nerve demonstrates a complete dropout of the outer retinal structures and absence of normal optic nerve head glial tissues distal to the papillomacular bundle.
Differential Diagnosis:
- Optic nerve pit
- Morning glory anomaly
- Advanced glaucoma
- Peripapillary central serous chorioretinopathy
- Colobomatous optic disc anomaly
- Discussion:
- Chorioretinal Colobomas
Colobomas of the optic nerve, retina, and choroid occur due to incomplete closure of the embryonic fissure in the fifth week of development. These colobomatous malformations appear to confer some increased risk of retinal detachments with 4-29% of colobomatous malformations resulting in retinal detachment.
Patients who develop retinal detachment are extremely unique cases that pose a challenge for management. Various techniques have been described, however none have proven to have a consistent results.
In light of the patient’s particular anatomy with an epiretinal membrane causing traction on the fovea, it was decided to complete a pars plana vitrectomy, membrane peeling, focal laser, and air tamponade.
The surgery was successful in collapsing the schisis cavity and flattening the macula.
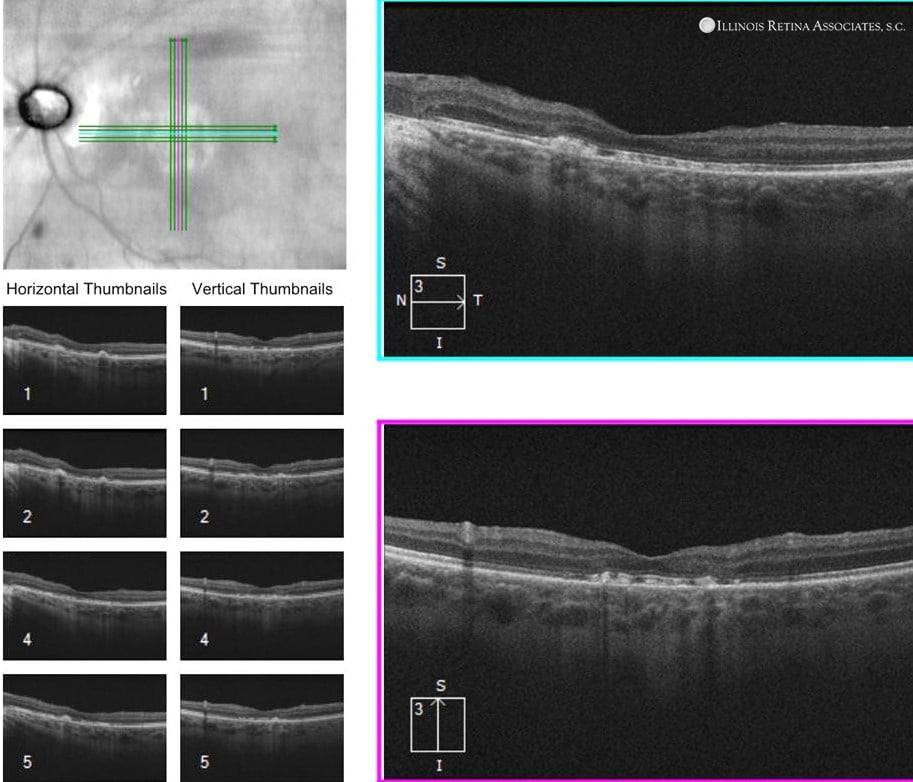
Figure 5. Post-operative OCT shows resolution of the retinal detachment.
Remarkably, the patient has maintained her 20/30 vision. Given the exceedingly rare nature of this disease, it is challenging to draw conclusions as to the best approach to address this disease. Hence, when the diagnosis of a posterior coloboma is suspected, a referral to a retina specialist may be valuable in prevention and treatment of such sequelae.
If you are looking to schedule your first consultation, please contact us today by clicking HERE and find the location that is nearest you!
References:
- Schubert H.D. Structural organization of choroidal colobomas of young and adult patients and mechanism of retinal detachment. Trans Am Ophthalmol Soc. 2005; 103: 457-472.
- Daufenbach D.R., Ruttum M.S., Pulido J.S., Keech R.V. Chorioretinal colobomas in a pediatric population. Ophthalmology. 1998; 105: 1455-1458.
- Maumenee I.H., Mitchell T.N. Colobomatous malformations of the eye. Trans Am Ophthalmol Soc. 1990; 88 (discussion 133-135): 123-132.
- Morrison D.A., Fleck B. Prevalence of retinal detachments in children with chorioretinal colobomas. Ophthalmology. 1999; 106: 645-646.

