Foveal Cavitation – August, 2022

History:
A 65-year-old female presents as a new patient referral for decreased vision. She has complaints of difficulty seeing at a distance for some time and feels like she needs stronger glasses. She has a history of radial keratotomy in both eyes about 20 years prior. She has no significant past medical history and takes Vitamin D supplements daily as her only medication. Her review of symptoms and her family history is also noncontributory.
Exam:
Her visual acuity is 20/60 in the right eye and 20/70 in the left eye. Her pupils are normally reactive without RAPD. Her intraocular pressure is 21 and 20 in right and left eye, respectively. Anterior segment exam was significant for radial keratotomy scars and mild nuclear cataract in both eyes. Her dilated exam was significant for a blunted foveal reflex in both eyes. Peripherally, her right eye showed small hypopigmented lesions temporally.
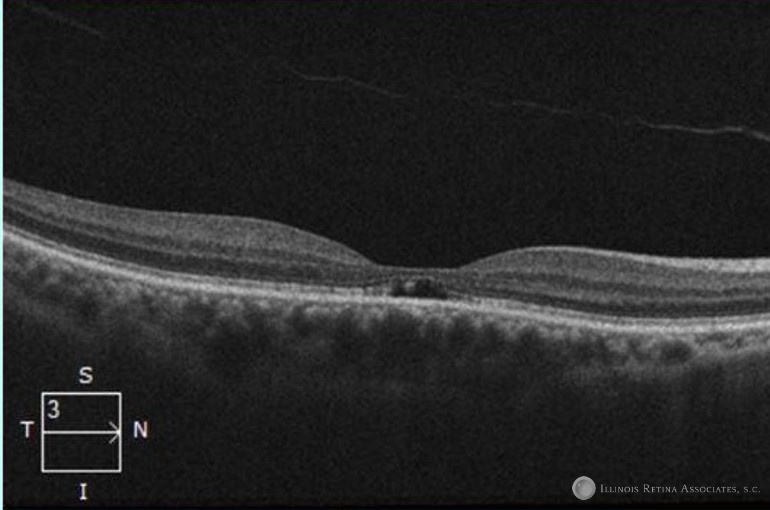
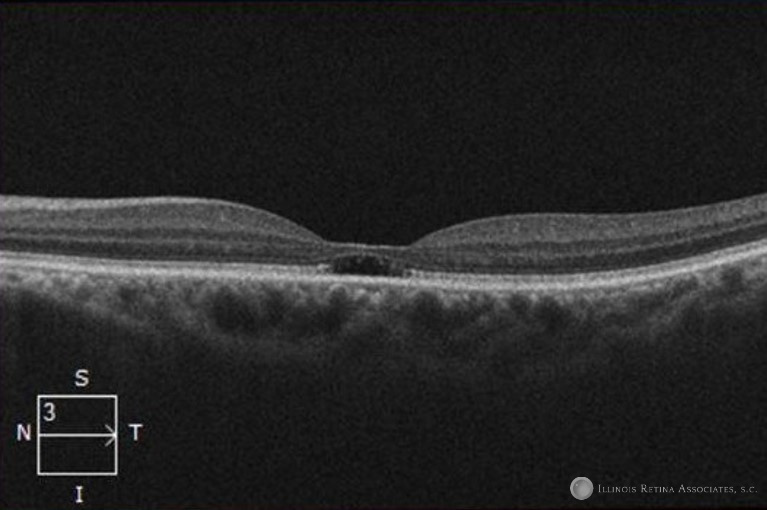
Figure 1: Optical Coherence Tomography (OCT) shows subfoveal disruption of inner segment/outer segment (IS/OS) layer consistent with foveal cavitations.
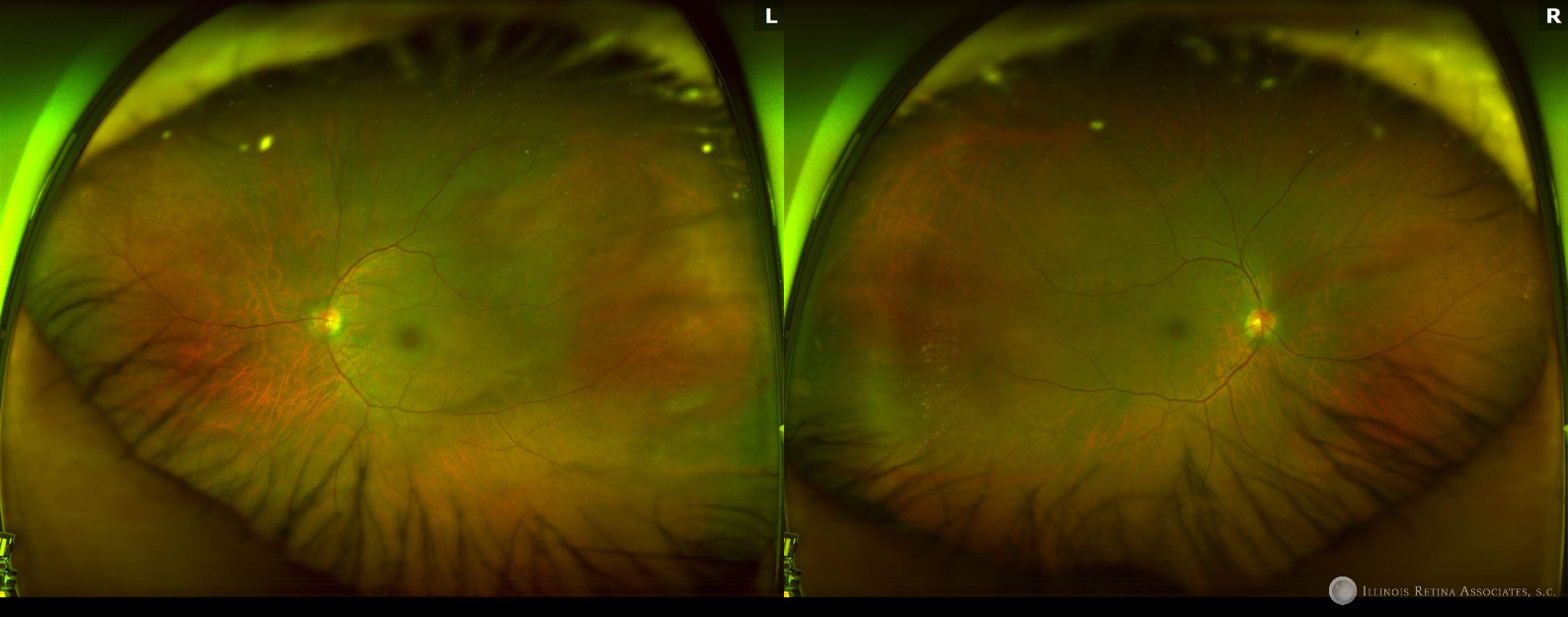
Figure 2: Fundus photographs of both eyes showing a small cluster of hypopigmented lesions in the right eye temporally. Both eyes show a blunted foveal reflex.
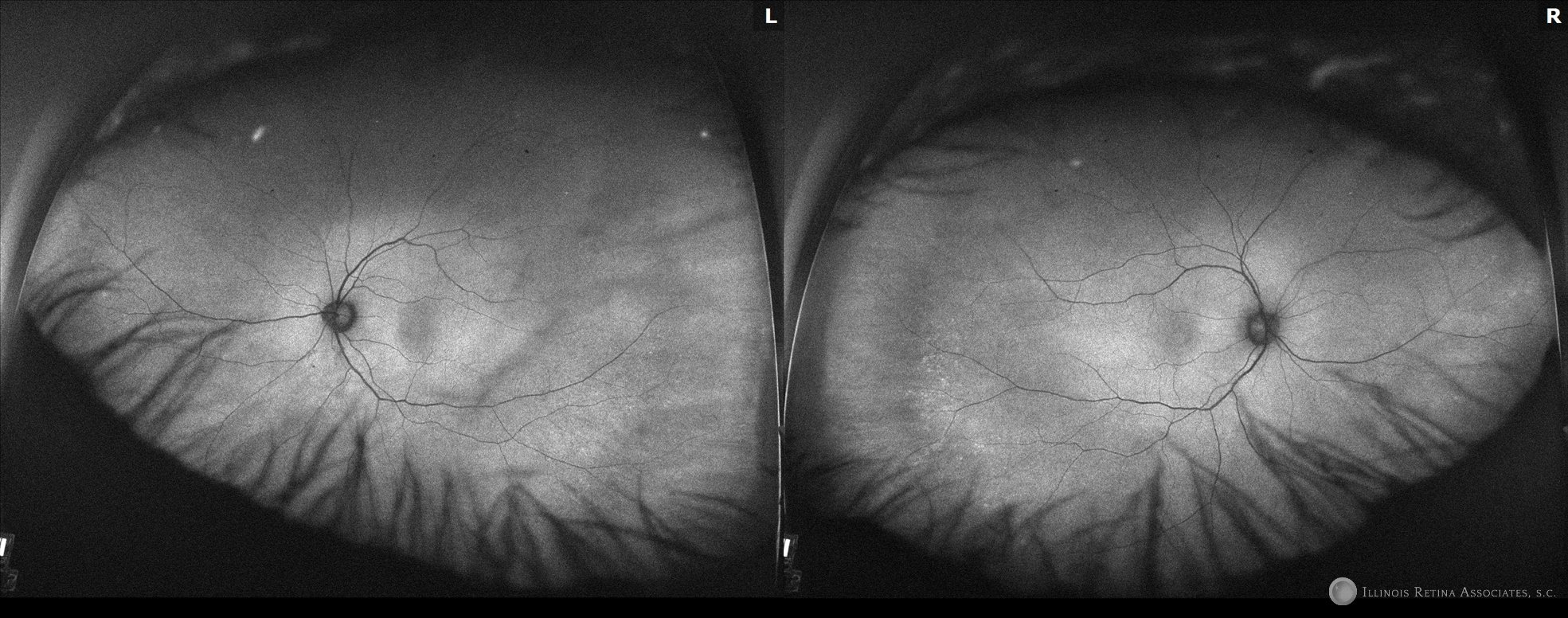
Figure 3: Autofluorescence of both eyes showing hypo-autofluorescence of the fovea in both eyes. The right eye showed a cluster of hyper-autofluorescence temporally.
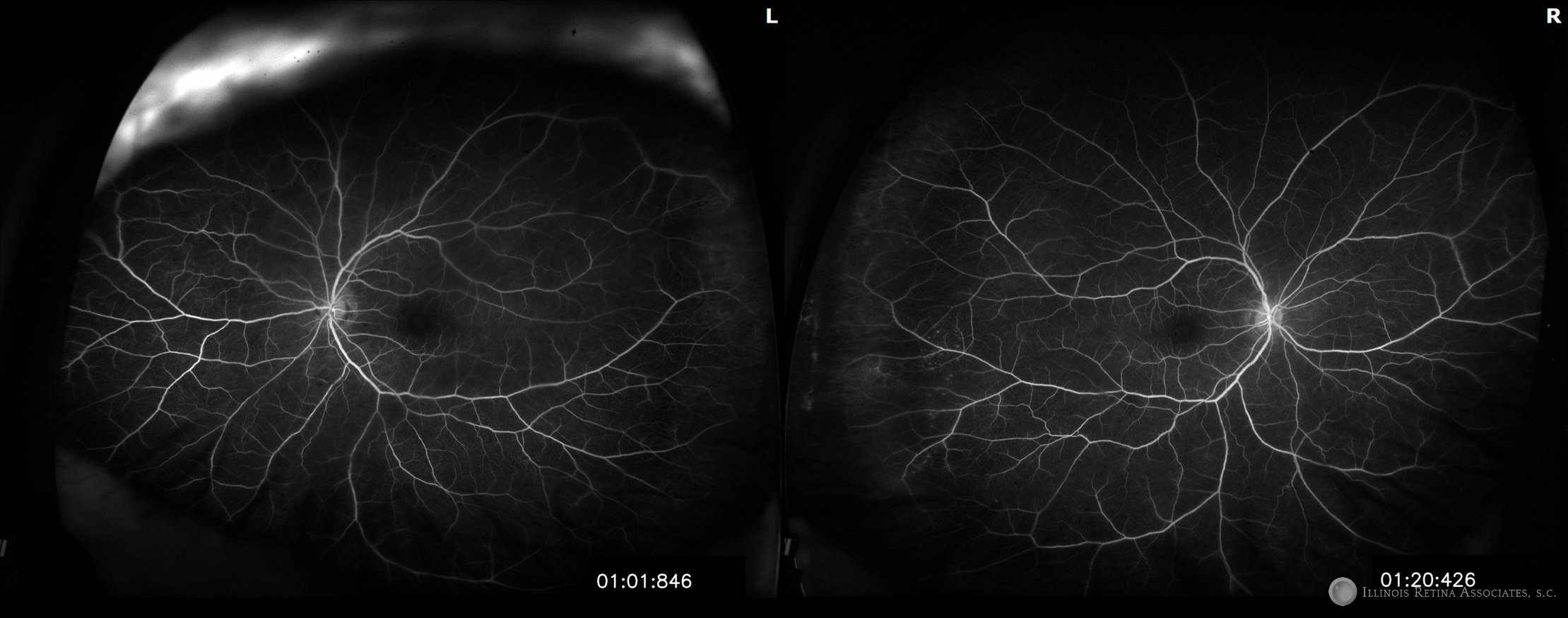
Figure 4: Fluorescein angiogram of both eyes showed normal transit times without leakage in the posterior pole.
An ERG was completed and showed rod receptor dysfunction and abnormal dark adaptation. Multifocal ERG was consistent with normal cone function.
Differential Diagnosis:
- Cone-rod dystrophy
- Solar maculopathy
- Tamoxifen use
- Occult macular dystrophy
- Stargardt disease
- Achromatopsia
Discussion:
Foveal Cavitations
Foveal cavitations have been described in multiple processes that are typically caused by cone dysfunction, including, but not limited to, cone-rod dystrophies, tamoxifen use, solar maculopathy, occult macular dystrophy, achromatopsia, and Stargardt disease. The foveal cavitation is characterized by loss of outer retinal layers, particularly the IS/OS junction, leaving an optically empty space. This space can be confused with subretinal fluid but is more of an optical gap within the outer retina.
Foveal cavitation was defined by Parodi et al. as loss of outer retinal layers, except for retinal pigment epithelium, with the preservation of the external limiting membrane. Incomplete foveal cavitation was also defined as partial disruption of the outer retinal layers. There was noted to be a statistically significant difference in vision between complete and incomplete foveal cavitation leading the authors to conclude that greater foveal cavitation leads to worse functional outcomes for the patient. It was specifically noted that the height of the cavitation and the distance from the RPE to the inner retinal layers correlated with worse visual acuity.
At this time, studies have not shown significant progression of foveal cavitation. Multiple authors have hypothesized that the variable outer retinal layer loss is due to variable cone dysfunction rather than early disease that will progress to further loss. Moving forward, it is possible this finding on OCT may be a key monitoring finding for treatment of these retinal dystrophies.
Our patient underwent genetic testing and was found to have a heterozygous mutation for FLVCR1. This gene is associated with autosomal recessive posterior column ataxia with retinitis pigmentosa. This finding, in addition to her ERG abnormalities, led us to conclude that she likely has some penetrance of this gene leading to her visual complaints and OCT findings. She is scheduled to return for follow up imaging and visual field testing.
If you are looking to schedule your first consultation, please contact us today by clicking HERE and find the location that is nearest you!
References:
- Leng, Theodore MD, MS; Marmor, Michael F. MD; Kellner, Ulrich MD; Thompson, Dorothy A. PhD; Renner, Agnes B. MD; Moore, William FRCS; Sowden, Jane C. PhD, FOVEAL CAVITATION AS AN OPTICAL COHERENCE TOMOGRAPHY FINDING IN CENTRAL CONE DYSFUNCTION, Retina: July 2012, Volume 32, Issue 7, p.1411-1419 doi:10.1097/IAE.0b013e318236e4ea
- Oh JK, Ryu J, Lima de Carvalho JR Jr, Levi SR, Lee W, Tsamis E, Greenstein VC, Mahajan VB, Allikmets R, Tsang SH. Optical Gap Biomarker in Cone-Dominant Retinal Dystrophy. Am J Ophthalmol. 2020 Oct;218:40-53. doi: 10.1016/j.ajo.2020.05.016. Epub 2020 May 21. PMID: 32445700; PMCID: PMC8291221.
- Parodi MB, Cicinelli MV, Iacono P, Bolognesi G, Bandello F. Multimodal imaging of foveal cavitation in retinal dystrophies. Graefes Arch Clin Exp Ophthalmol. 2017 Feb;255(2):271-279. doi: 10.1007/s00417-016-3450-7. Epub 2016 Aug 5. PMID: 27491512.
- Rishi R. Doshi, Jorge A. Fortun, Brian T. Kim, Sander R. Dubovy, Philip J. Rosenfeld, Pseudocystic Foveal Cavitation in Tamoxifen Retinopathy, American Journal of Ophthalmology, Volume 157, Issue 6, 2014, Pages 1291-1298.e3, ISSN 0002-9394, https://doi.org/10.1016/j.ajo.2014.02.046.

