Macular Telangiectasia – April 2017

Case Presentation
A 54 year-old female was referred to Illinois Retina Associates for decreased vision and macular changes in both eyes. Her visual symptoms had been present for 5 years, but progressively worsening. She had no past ocular history.
She was known for back pain and elbow epicondylitis and taking the following medication: gabapentin, naproxen, alprazolam, fluoxetine.
Examination
Her uncorrected visual acuity was 20/50 in the right eye, and 20/100 in the left eye, not improved with pinhole. Anterior segment examination showed nuclear sclerosis in both eyes. On posterior segment examination, there was a gray appearance and pigment mottling in the temporal part of the macula in both eyes and the loss of foveal reflex (Figures 1 & 2).
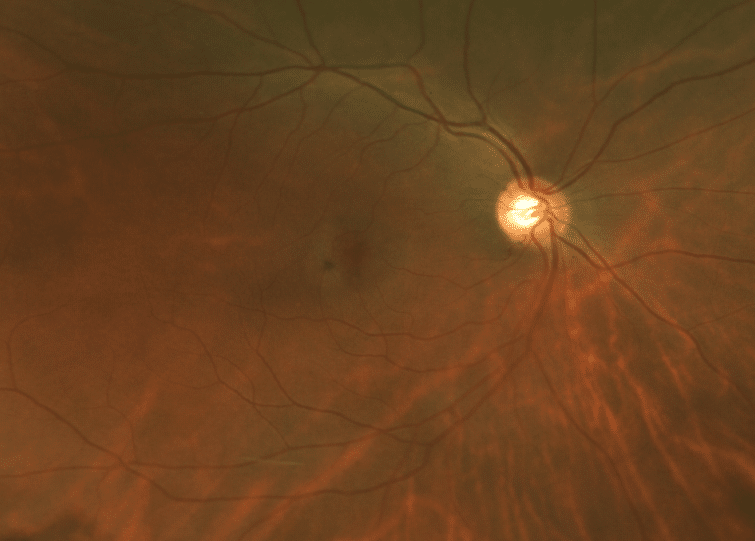
Figure 1
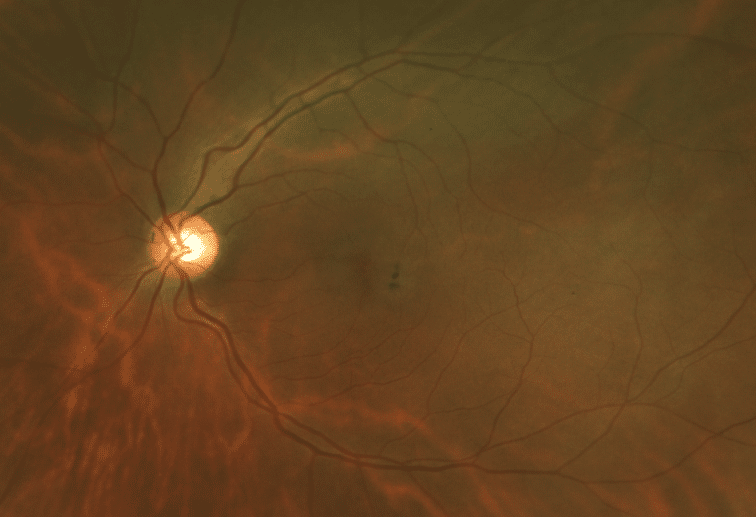
Figure 2
Differential Diagnosis
-
Macular Degeneration - Macular Dystrophy
- Focal Laser Scarring
- Epiretinal Membrane
- Photic/Solar Maculopathy
- Macular Telangiectasis
- Toxic Maculopathy (Plaquenil)
Diagnostic Testing
On fundus autofluorescence imaging, there was increased autofluorescence in the foveal region of each macula and focal hypoautofluorescence corresponding to the pigment mottling (Figures 3 & 4). Fluorescein angiography showed hyperfluorescence due to leaking telangiectatic vessels around the fovea, more on the temporal side (Figures 5 & 6). Optical coherence tomography showed small foveal cystoid cavities, disorganized retinal layers on the temporal side, and pigment migration into the retina (Figures 7 & 8).
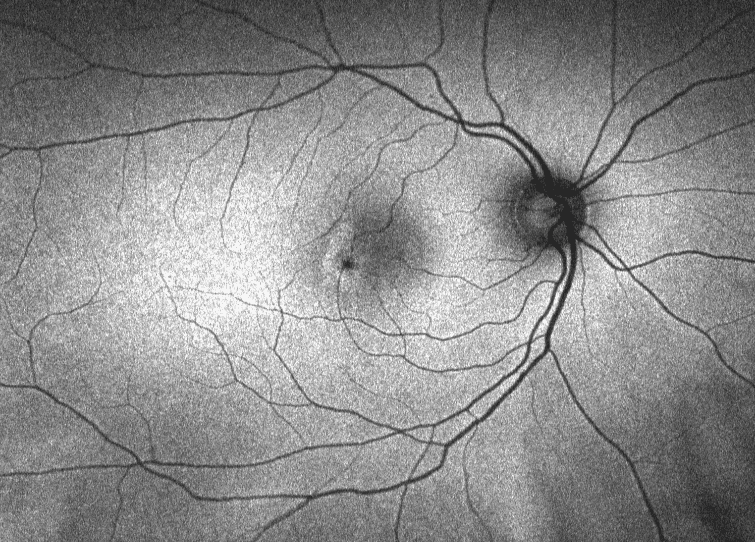
Figure 3

Figure 4
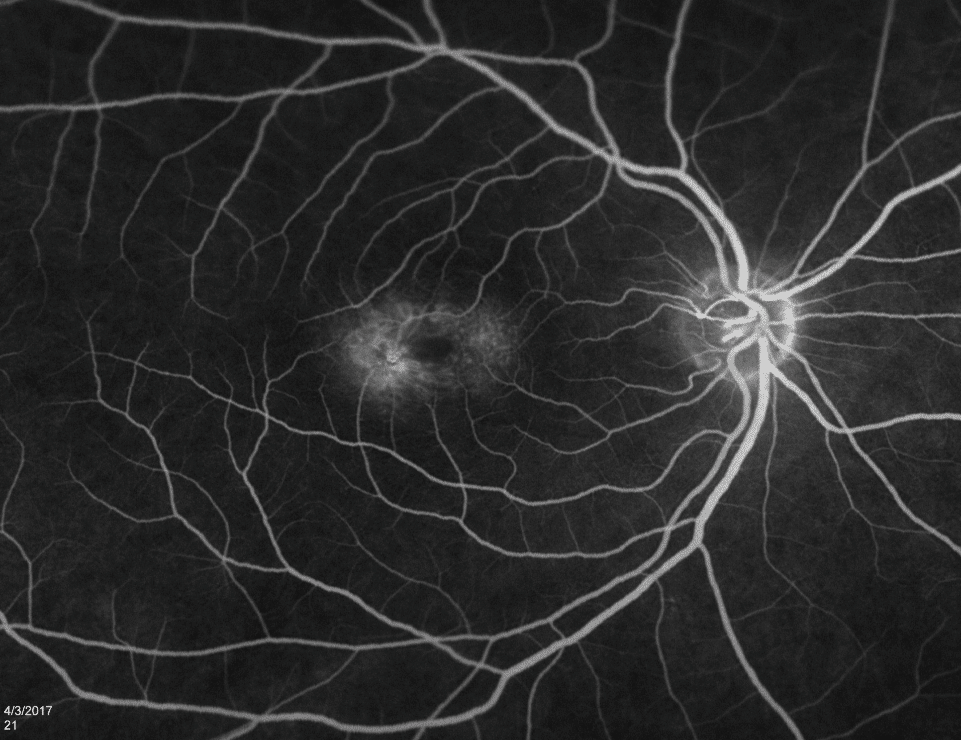
Figure 5
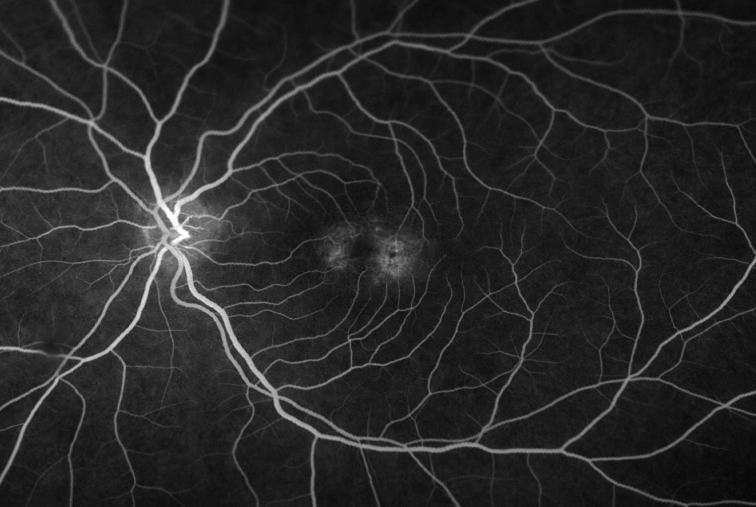
Figure 6
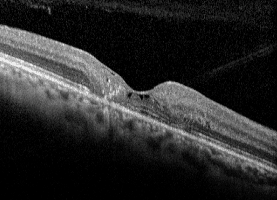
Figure 7
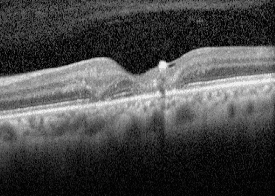
Figure 8
Diagnosis
Macular telagiectasis, also called idiopathic juxtafoveal telangiectasis, is typically subdivided into 3 subtypes, depending on their presentation. Type 1 is unilateral and is associated with parafoveal capillary dilation, microaneurysms and lipid exudation. Type 2 is the most common, is bilateral, and does not present with lipid. Type 3 is very rare and is characterized by parafovea ischemia.
Macular telangiectasis type 2 most commonly presents in middle age, has no gender nor racial predilection and is not inherited. Common complaints include blurry vision, distortion and scotomas.
Imaging studies, including autofluorescence, fluorescein angiography and OCT can be helpful in making the diagnosis early, when findings may be subtle. Some early findings include graying of the retina, telangiectasias, crystalline deposits, right-angle venules and cystoid spaces.
Patients are at risk of developing subretinal neovascularization with a subsequent rapid decrease in vision. There is no proven treatment for the nonproliferative stage, but once neovascularization is present, it may respond well to anti-VEGF injections.
The disease tends to have a slowly progressive course in the majority of patients, with visual loss over time.
References
Cohen SM, Cohen ML, El-Jabali F, Pautler SE. Optical coherence tomography findings in nonproliferative group 2a idiopathic juxtafoveal retinal telangiectasis Retina 2007:27(1):59-66
Gass JD, Blodi BA. Idiopathic juxtafoveolar retinal telangiectasis. Update of classification and follow-up study. Ophthalmology 1993;100(10):1536-46
Nowilaty SR, Al-Shamsi HN, Al-Khars W. Idiopathic juxtafoveolar retinal telangiectasis: a current review Middle East Afr J Ophthalmol 2010;17(3):224-41
Roller AB, Folk JC, Patel NM, Boldt HC, Russel SR, Abramoff MD, Mahajan VB Intravitreal bevacizumab for treatment of proliferative and nonproliferative type 2 idiopathic macular telangiectasia Retina 2011;31(9):1848-55
Watzke RC, Klein ML, Folk JC, Farmer SG, Munsen RS, Champfer RJ, Sletten KR. Long-term juxtafoveal retinal telangiectasia Retina 2005;25(6):727-35
Wong WT, Forooghian F, Majumdar Z, Bonner RF, Cunningham D, Chew EY Fundus autofluorescence in type 2 idiopathic macular telangiectasia: correlation with optical coherence tomography and microperimetry. Am J Ophthalmol 2009;148(4):573-83
Yannuzi LA, Bardal AM, Freund KB, Chen KJ, Eandi CM, Blodi B. Idiopathic macular telangiectasia. Arch Ophthalmol 2006;124(4)450-60

