Ocular Ischemic Syndrome (OIS) – June, 2023

History:
A 68-year-old male presented with blurred vision in the right eye for 1-2 months. He had recently had a stroke which left him with left sided weakness. He reported his stroke was due to an embolism. He has a history of hypertension and is a current smoker. He reported no issues with his left eye.
Exam:
His visual acuity was 20/200 in the right eye which improved to 20/50 with pinholes. Vision in the left eye was 20/20. His right pupil was minimally reactive but there is no RAPD. His color vision was significantly altered with 0/15 color plates in the right eye. Anteriorly, he had 1+ flare and 2+ nuclear sclerosis in the right eye. The left eye was normal. Dilated fundus exam showed multiple dot blot hemorrhages in the macula and midperiphery in the right eye.
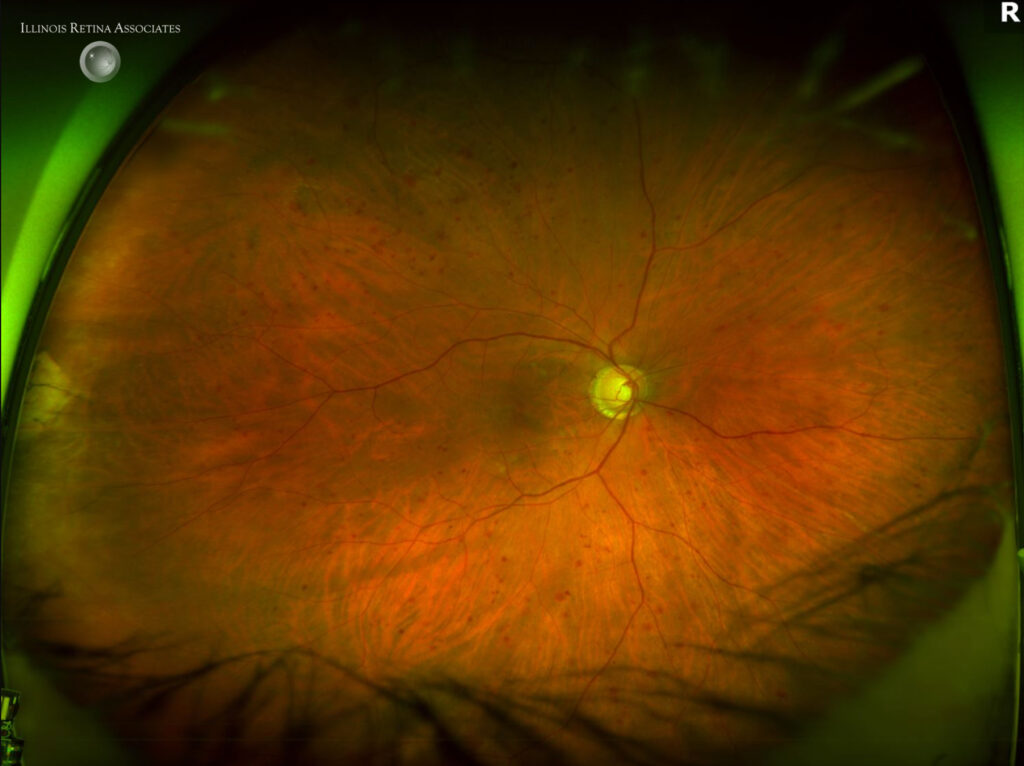
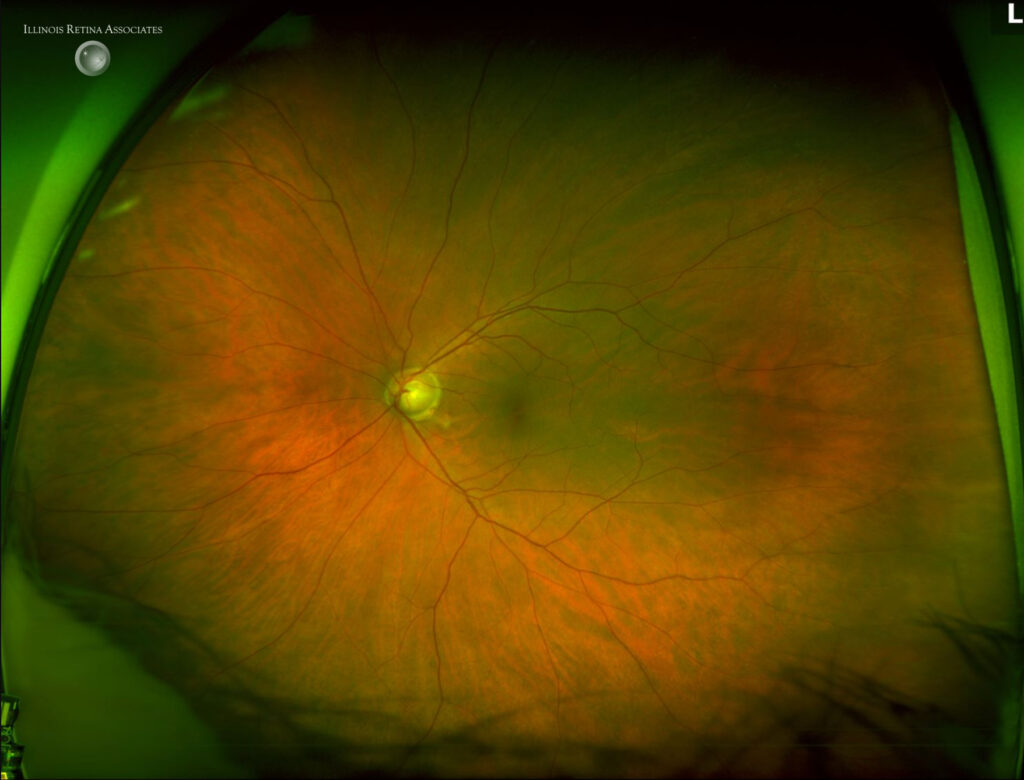
Figure 1a and 1b: Fundus photography of both eyes showed numerous dot blot hemorrhages in the right eye and normal fundus in the left eye.
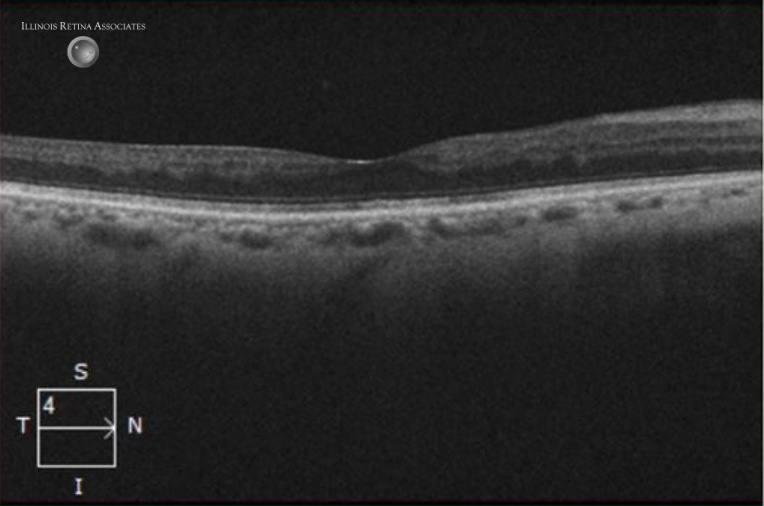
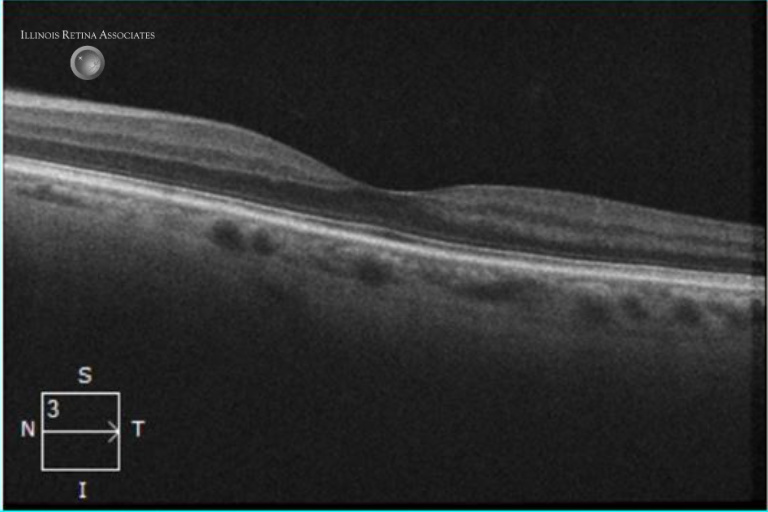
Figure 2a and 2b: Optical coherence tomography (OCT) retina showed diffuse retinal thinning in the right eye and normal scan in the left eye.
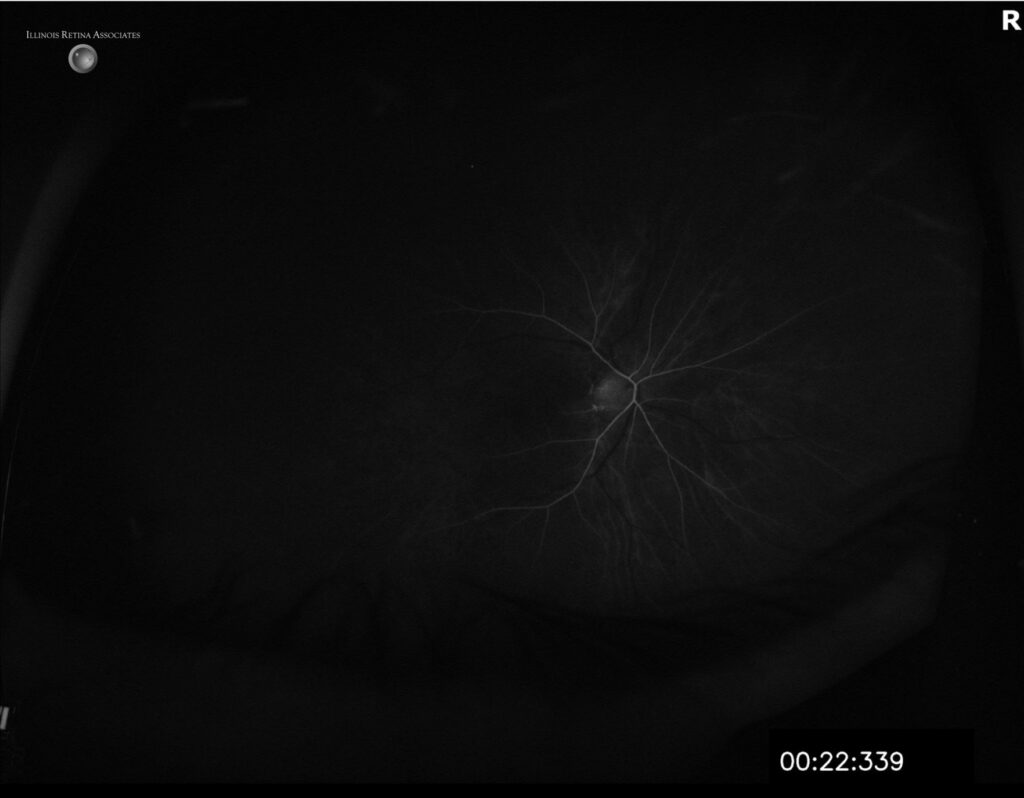
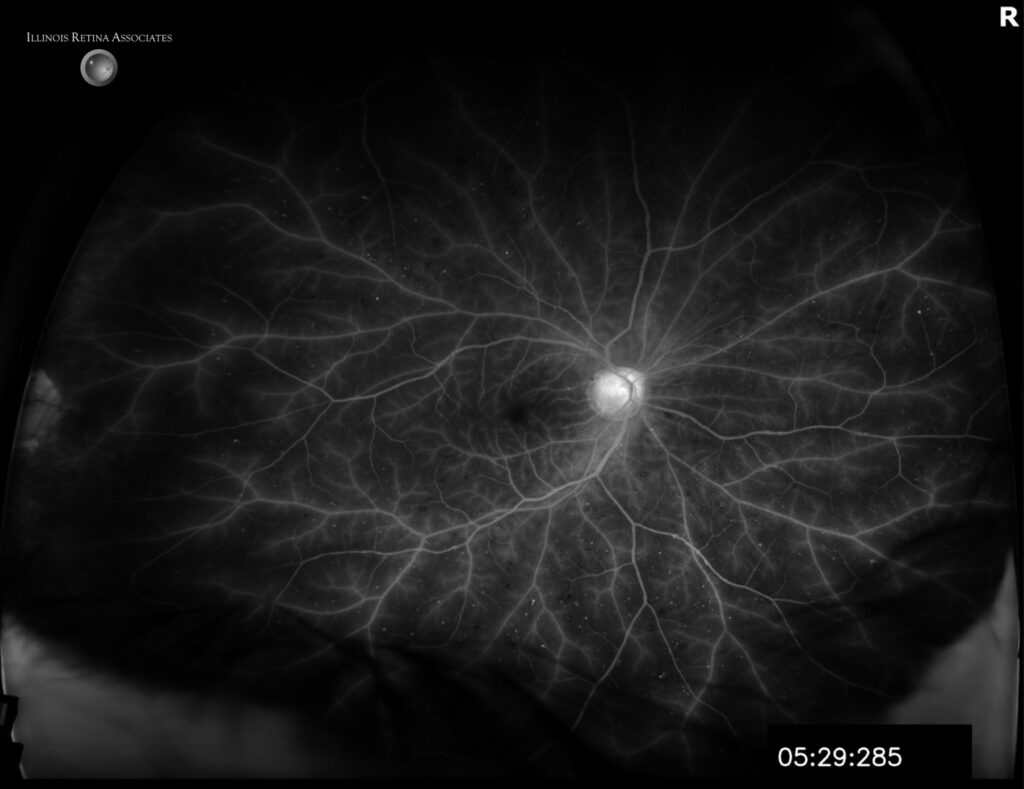
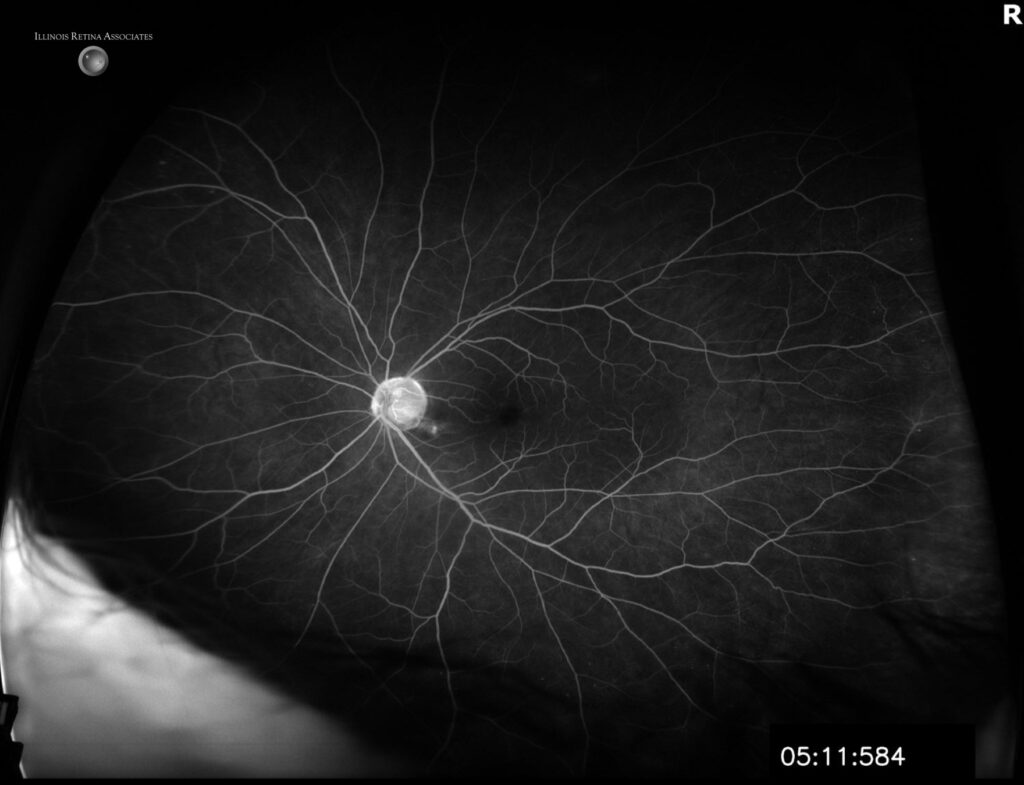
Figure 3a, 3b and 3c: Fluorescein angiogram (FA) showed significantly delayed filling in the right eye with late vascular leakage. The left eye only showed very mild peripheral microaneurysms.
Differential Diagnosis:
-
Central retinal vein occlusion - Diabetic retinopathy
- Hypertensive retinopathy
- Ocular ischemic syndrome
- Hyperviscosity syndromes
Discussion:
Ocular Ischemic Syndrome (OIS)
During workup for his stroke, the patient was found to have nearly complete occlusion of the right carotid artery. The patient later developed neovascular glaucoma with neovascularization of the iris and elevated IOP. He was treated with anti-VEGF to control the IOP and NVI. PRP was then completed in the right eye only. The patient’s vision dropped to 20/100 and has remained stable for years without new neovascularization.
Ocular ischemic syndrome (OIS) can often be confused with central retinal vein occlusion or diabetic retinopathy as these patients often have the same or similar risk factors. OIS often presents with dilated venules, dot blot hemorrhages in the mid periphery, midperipheral microaneurysms, no hard exudates, and normal appearing optic nerve. The FA will show delayed transit time, late staining of arteries more than veins, patchy or delayed choroidal filling, and mid peripheral microaneurysms.
OIS is often associated with and may be the presenting finding of severe carotid atherosclerosis. The stroke rate in patients with OIS is significantly higher, 4% per year, compared to 0.49% per year in patients without OIS. Patients need to be counseled on this risk and communication of this diagnosis to the patient’s PCP and/or neurologist is imperative. Lifestyle modifications, including weight loss and smoking cessation, are also important. In patients without carotid artery disease, other arteritis syndromes should be considered such as giant cell arteritis (GCA), aortic arch syndrome, Takayasu arteritis, carotid artery dissection, hyperhomocysteinemia, radiotherapy of the neck with carotid occlusion, thyroid orbitopathy, Moyamoya disease, neurofibromatosis, and scleroderma.
Ocular treatment for OIS targets decreasing retinal ischemia and neovascular glaucoma. Topical treatments to decrease anterior segment inflammation and cycloplegia to limit iris movement can decrease the rate of spontaneous hyphema. Medical treatment for IOP control is also used. Prostaglandins and pilocarpine should be avoided, if possible, due to their pro-inflammatory characteristics. Intravitreal anti-VEGF and PRP can be used to treat neovascularization.
If you are looking to schedule your first consultation, please contact us today by clicking HERE and find the location that is nearest you!
References:
-
Gordon N. Ocular manifestations of internal carotid artery occlusion. The British journal of ophthalmology. May 1959;43(5):257-267. - Mendrinos E, Machinis TG, Pournaras CJ. Ocular ischemic syndrome. Survey of ophthalmology. Jan-Feb 2010;55(1):2-34.
- Goldstein LB, Adams R, Alberts MJ, et al. Primary prevention of ischemic stroke: a guideline from the American Heart Association/American Stroke Association Stroke Council: cosponsored by the Atherosclerotic Peripheral Vascular Disease Interdisciplinary Working Group; Cardiovascular Nursing Council; Clinical Cardiology Council; Nutrition, Physical Activity, and Metabolism Council; and the Quality of Care and Outcomes Research Interdisciplinary Working Group. Circulation. Jun 20 2006;113(24):e873-923.

